Your gut health directly impacts your metabolism. An imbalanced gut microbiome, or dysbiosis, can lead to inflammation, insulin resistance, and weight gain - all contributors to metabolic disorders like type 2 diabetes and obesity. Postbiotics, the inactive byproducts of beneficial bacteria, offer a solution by improving insulin sensitivity, reducing inflammation, and supporting gut barrier function. Unlike probiotics, postbiotics don’t require live bacteria to work, making them effective and stable for immediate metabolic benefits.
Key Takeaways:
- Gut Imbalance: Linked to chronic inflammation, insulin resistance, and metabolic endotoxemia.
- Postbiotics Role: Improve glucose regulation, manage appetite, and reduce inflammation.
- Clinical Evidence: Studies show reduced insulin levels, lower triglycerides, and smaller waist circumference with postbiotic use.
- Modern Lifestyle Factors: Diets high in fats and sugars, antibiotics, and poor sleep harm gut health.
- Synbiotic Solutions: Combining prebiotics, probiotics, and postbiotics can restore gut balance effectively.
Postbiotics are a promising tool to address metabolic health challenges by targeting the root causes of gut imbalance.
How Gut Imbalance Contributes to Metabolic Disorders
Mechanisms of Metabolic Disruption from Dysbiosis
When your gut microbiome falls out of balance - a condition called dysbiosis - it can spark a chain reaction of metabolic issues. One key pathway is metabolic endotoxemia, which occurs when a high-fat diet weakens your intestinal barrier. This allows bacterial lipopolysaccharides (LPS) from gram-negative bacteria to leak into your bloodstream. Once there, LPS activates Toll-like receptors, triggering low-grade systemic inflammation that disrupts insulin sensitivity [9][10]. This is a prime example of how lifestyle choices can amplify gut imbalances.
Your gut microbiota also plays a major role in energy extraction from food. For instance, in Western diets, microbial fermentation of complex carbohydrates into short-chain fatty acids contributes to about 10% of total absorbed energy [4]. Dysbiosis can upset this process - beneficial butyrate levels drop, while harmful bacteria that extract excessive calories thrive. Studies even show that introducing microbiota to germ-free mice can cause a 60% increase in body fat and insulin resistance within just two weeks, even when their food intake is reduced [4][10].
Another way dysbiosis affects your metabolism is through toxic byproducts. Certain microbes, like Prevotella copri, produce high levels of branched-chain amino acids (BCAAs), which are strongly linked to insulin resistance [7]. Gut bacteria can also convert dietary choline into trimethylamine, which the liver turns into TMAO - a compound associated with increased risks of diabetes and heart disease [7][9]. Additionally, individuals with insulin resistance often have higher levels of fecal monosaccharides, such as fructose and mannose, which correlate with elevated inflammatory markers [8].
"Events that start in the gut, often in response to external cues such as diet and circadian disruption, have far-reaching effects beyond the gut." - Kruttika Dabke, Gustaf Hendrick, and Suzanne Devkota, Cedars-Sinai Medical Center [9]
Modern Lifestyle Factors That Damage Gut Health
External factors, especially those tied to modern lifestyles, can worsen gut health and exacerbate metabolic issues. Your daily habits have a profound impact on your microbiome. For example, Western diets, which are heavy in refined sugars, processed foods, and saturated fats, encourage the growth of harmful bacteria while suppressing beneficial ones. Switching to an animal-based diet - rich in meats, eggs, and cheeses - can cause a spike in bile-tolerant microbes like Bilophila wadsworthia in as little as five days [9]. High-fat diets can also disrupt the microbiome's natural circadian rhythm, which interferes with the liver’s ability to regulate fatty acid and glucose metabolism [9].
Another major disruptor is antibiotic overuse, which can have long-lasting effects on your gut microbiota. Broad-spectrum antibiotics, in particular, deplete butyrate-producing bacteria that are crucial for glucose regulation [4][10]. Other factors, like lack of exercise, chronic stress, and poor sleep, also destabilize your gut microbiome. These lifestyle issues contribute to the alarming rise in metabolic disorders. Today, over 800 million adults worldwide are living with diabetes - a number that has more than quadrupled since 1990 [11].
While genetics influence microbiome composition to some extent, environmental factors are far more impactful. Only 10%–20% of microbial variation is linked to host genetics [11]. The good news? Even small dietary changes can shift your gut microbiota within just a few hours or days [11], offering a chance to restore balance and improve overall health.
How Postbiotics Improve Metabolic Health
What Postbiotics Are
Postbiotics bring a fresh perspective to gut health. According to the International Scientific Association for Probiotics and Prebiotics (ISAPP), they are defined as "a preparation of inanimate microorganisms and/or their components that confers a health benefit on the host" [12][13]. Unlike probiotics, which rely on surviving stomach acid and colonizing the gut, postbiotics are ready to work immediately upon consumption.
Their makeup includes inactive microbial cells, cell wall fragments (like peptidoglycans and teichoic acid), and bioactive compounds such as short-chain fatty acids (SCFAs), enzymes, peptides, and vitamins [12][3][5]. These components are the active agents delivering metabolic benefits, eliminating the need for further activation.
Postbiotics offer practical advantages. They are shelf-stable, resistant to heat, and avoid risks like bacterial translocation or spreading antibiotic-resistance genes [13][15]. Unlike many probiotics, which can lose viability during storage, postbiotics don’t require refrigeration [13][15]. This makes them a safer option for individuals with weakened immune systems [13][14]. When shopping for postbiotics, look for terms like "heat-killed", "tyndallized", or "bacterial lysate" on the label to confirm you're getting authentic postbiotic ingredients [13][17].
"Postbiotics can be more effective than probiotics, as they don't require prebiotic fibers to be present... some people don't tolerate live probiotics due to significant dysbiosis of the gut, so postbiotics can be more effective with less side effects." - Heather Moday, MD, Functional Medicine Physician [15]
By understanding their bioactive components, it's easier to appreciate how postbiotics affect metabolic health.
The Science of Postbiotics and Metabolism
Postbiotics support metabolic health through multiple mechanisms. One key pathway involves hormonal signaling. SCFAs activate receptors like GPR41 and GPR43 in the gut, which stimulate the release of appetite-regulating hormones such as GLP-1 and PYY [3][5]. This not only helps control hunger but also enhances glucose management across the body.
Another critical role of postbiotics is activating AMPK, a metabolic regulator that boosts fatty acid breakdown while reducing fat production [16]. This dual impact helps address metabolic imbalances. Clinical studies highlight the measurable benefits: postbiotic supplementation has been shown to lower serum insulin by an average of 2.76 µU/mL, reduce triglycerides by 8.46 mg/dL, and shrink waist circumference by 1.47 cm [5].
Inflammation, a common factor in metabolic disorders, is another target for postbiotics. They reduce inflammatory markers like TNF-α and IL-6, while also decreasing C-reactive protein (CRP) levels by 0.99 mg/L [3][5]. By strengthening the intestinal barrier and preventing the leakage of bacterial toxins (a condition known as metabolic endotoxemia), postbiotics tackle one of the root causes of insulin resistance. For noticeable results, interventions typically need to last longer than 8 weeks [5].
Prebiotics, Probiotics, and Postbiotics Explained | Dr. Will Bulsiewicz
sbb-itb-1bbfe7f
Clinical Evidence for Postbiotics and Metabolic Health
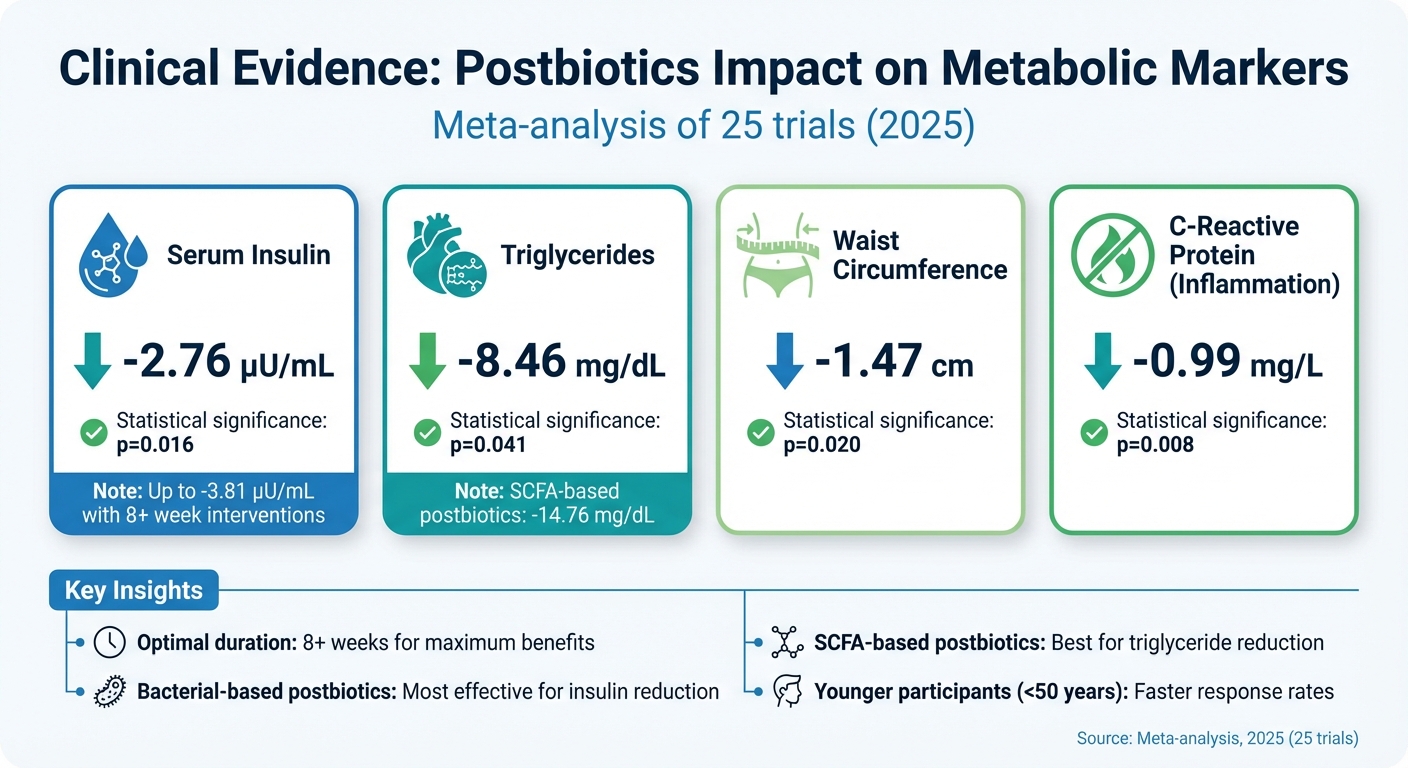
Clinical Evidence: How Postbiotics Improve Metabolic Health Markers
Research Results on Metabolic Markers
A meta-analysis from 2025, covering 25 trials, highlights the positive impact of postbiotics on metabolic health. Participants in these studies saw an average serum insulin reduction of 2.76 µU/mL, pointing to better insulin sensitivity. Triglyceride levels also dropped by 8.46 mg/dL, and waist circumference - a critical measure of visceral fat - decreased by 1.47 cm. Additionally, inflammation markers showed improvement, with C-reactive protein (CRP) levels falling by 0.99 mg/L. Notably, interventions lasting 8 weeks achieved insulin reductions of up to 3.81 µU/mL [5].
| Metabolic Marker | Improvement | Statistical Significance |
|---|---|---|
| Serum Insulin | -2.76 µU/mL | p=0.016 |
| Triglycerides | -8.46 mg/dL | p=0.041 |
| Waist Circumference | -1.47 cm | p=0.020 |
| C-reactive Protein | -0.99 mg/L | p=0.008 |
Further analysis revealed that different types of postbiotics target specific markers. For instance, bacterial-based postbiotics are particularly effective at reducing insulin levels, while SCFA-based postbiotics can lower triglycerides by as much as 14.76 mg/dL. Younger participants, especially those under 50, tend to respond more rapidly to these interventions [5].
Why Postbiotics Deliver Consistent Results
The effectiveness of postbiotics stems from their inherent molecular stability, which ensures reliable results. Unlike probiotics, postbiotics remain functional without refrigeration, tolerating temperature changes without losing potency. This stability guarantees the consistent delivery of bioactive compounds, which interact with receptors like GPR41 and GPR43 to regulate appetite hormones and glucose metabolism [5][6][1][16].
Postbiotics also offer practical advantages. Their stability allows for easier handling, storage, and transport, making them more cost-effective compared to probiotics. For example, research on pasteurized Akkermansia muciniphila demonstrated that the inactivated form was more effective at improving insulin resistance than its live counterpart. This highlights how non-living bacterial components can reliably support metabolic health by targeting key pathways [1][3].
These findings emphasize the role of postbiotics in addressing metabolic dysfunction, offering a stable and effective tool for improving health outcomes.
Synbiotic Formulations: Combining Prebiotics, Probiotics, and Postbiotics
How Synbiotics Restore Gut Balance
Synbiotics bring together three powerful components: prebiotic fibers (like inulin and GOS), live probiotics (such as Lactobacillus and Bifidobacterium), and bioactive postbiotics (like short-chain fatty acids and enzymes). Together, they tackle gut health from multiple angles. This approach creates a synergistic effect, where the prebiotic fibers are specifically designed to nourish the probiotics they’re paired with. This targeted combination often works better than using any single component on its own. For instance, synbiotic blends featuring Bifidobacterium lactis, Lactobacillus rhamnosus, and oligofructose-enriched inulin have been shown to regulate the gut environment more effectively than when these elements are used separately [2][18].
One key benefit of synbiotics is their ability to support the intestinal barrier. They do this by boosting tight-junction proteins like zonula occludens-1 (ZO-1) and occludin, which help prevent inflammatory compounds from leaking into the bloodstream - a condition linked to insulin resistance. At the same time, postbiotic short-chain fatty acids improve insulin sensitivity and enhance signals related to satiety. These combined actions create a comprehensive approach to reducing inflammation and improving metabolic health.
Begin Rebirth RE-1™: A Complete Microbiome Reset Solution
Building on these principles, Begin Rebirth RE-1™ offers a practical way to restore gut balance and support metabolic health. This advanced formulation utilizes the three-pronged synbiotic strategy to deliver measurable results.
Each sachet contains 500 billion CFU of HOSt™ probiotics, which are naturally adapted to the human gut, along with 4.5 grams of prebiotic fiber (GOS and inulin) and active postbiotic compounds.
The unique Lyosublime™ delivery system ensures these beneficial ingredients survive the harsh stomach environment, delivering probiotics and postbiotics directly to where they’re needed most. Unlike many probiotics that require refrigeration and may lose potency over time, this formulation stays stable at room temperature without compromising effectiveness. Flexible reset protocols - spanning 7 days, 4 weeks, or 12 weeks - allow users to address acute gut imbalances or work toward long-term microbiome health and sustained metabolic benefits.
Conclusion
Postbiotics provide bioactive compounds that support insulin sensitivity, reduce inflammation, and strengthen the intestinal barrier. Clinical trials have shown that postbiotics can improve key metabolic markers such as serum insulin, triglycerides, waist circumference, and C-reactive protein levels [5]. These benefits target core issues of metabolic dysfunction.
One of the standout features of postbiotics is their reliability. Unlike probiotics, which must survive stomach acid and establish themselves in the gut, postbiotics begin working as soon as they reach the digestive system. This dependability makes them a valuable tool for gut health. As Professor Tim Spector from King's College London explains:
"The recent discoveries that a dead microbe may be just as useful as a live one opens the door for innovative food products and more research... I now believe that postbiotics will be a mainstay in the future of functional food" [19].
For optimal results, postbiotics should be used for at least eight weeks, with longer usage leading to greater improvements in insulin sensitivity and waist circumference [5]. Formulations based on heat-inactivated bacteria, such as Lactobacillus or Bifidobacterium strains, tend to deliver better metabolic benefits compared to supplements containing only short-chain fatty acids (SCFAs) [5].
Building on these clinical findings, Begin Rebirth RE-1™ takes a comprehensive synbiotic approach by combining prebiotics, probiotics, and postbiotics to restore the microbiome effectively. Each daily sachet provides 500 billion CFU of Human Origin Strains, 4.5 grams of prebiotic fiber, and active postbiotic compounds. The Lyosublime™ delivery system ensures these ingredients reach the gut intact. Flexible reset protocols, ranging from 7 days to 12 weeks, allow you to customize your plan based on your metabolic health needs.
Gut restoration isn't just about temporary fixes - it's about laying the groundwork for lasting metabolic health. Incorporating postbiotics as part of a synbiotic strategy addresses inflammation, insulin resistance, and gut barrier issues at their root.
FAQs
What’s the difference between probiotics and postbiotics?
Probiotics are live microorganisms that can benefit your health when taken in the right amounts. They primarily help by interacting with or colonizing the gut microbiome, which supports both digestive and immune functions.
Postbiotics, on the other hand, are inactivated microorganisms or the beneficial compounds they produce. These include substances like metabolites, enzymes, and peptides, which can positively impact the body without involving live bacteria. Because they don’t contain live microbes, postbiotics are often a safer option for people with weakened immune systems.
While both probiotics and postbiotics contribute to gut health, they achieve this in different ways, each playing a unique role in promoting overall wellness.
How do postbiotics help improve insulin sensitivity and reduce inflammation?
Postbiotics, the compounds formed during microbial fermentation in the gut, play an important role in supporting insulin sensitivity and reducing inflammation. These substances help restore balance to the gut microbiome, addressing dysbiosis, a condition often tied to chronic inflammation and insulin resistance.
Here’s how they work: postbiotics help lower pro-inflammatory markers while encouraging anti-inflammatory activity, which can reduce overall systemic inflammation. They also have a positive effect on glucose regulation and lipid metabolism, which are essential for better insulin function. For instance, postbiotics may help decrease LDL cholesterol, triglycerides, and fasting blood sugar levels - all of which contribute to healthier metabolic function.
By focusing on gut health and reducing inflammation throughout the body, postbiotics show real promise in managing metabolic issues like diabetes and obesity.
What lifestyle habits can boost the effectiveness of postbiotics for better metabolic health?
Adopting healthy habits can amplify the impact of postbiotics on metabolic health. Start with a diet packed with fiber-rich foods, cut back on processed options, and stay active. These steps not only support your gut microbiome but also help postbiotics work more effectively. A balanced gut can play a big role in addressing metabolic concerns, including obesity and diabetes.
Stress management and limiting unnecessary antibiotic use are also key. Both help maintain a diverse gut microbiome, which is essential for postbiotics to do their job in regulating inflammation and metabolism. Adding prebiotic-rich foods like fruits, vegetables, and whole grains to your diet can further encourage the production of beneficial postbiotics.
For a more focused approach, consider products like Begin Rebirth RE-1™, a clinically-supported microbiome reset designed to restore gut balance and aid metabolic health. Pairing these lifestyle changes with targeted solutions can lead to even greater benefits.