Your gut and brain are deeply connected through the gut-brain axis, influencing mental health via neural, hormonal, and immune pathways. Prebiotics, probiotics, and postbiotics play key roles in this connection by improving gut health, which can impact mood, stress, and mental clarity.
- Prebiotics: Non-digestible fibers that feed gut bacteria, promoting the production of beneficial compounds like short-chain fatty acids (SCFAs). These can reduce stress and improve sleep quality.
- Probiotics: Live microorganisms like Lactobacillus and Bifidobacterium strains that produce neurotransmitters (e.g., serotonin, GABA) and reduce inflammation.
- Postbiotics: Inactive microbial components that deliver gut health benefits, strengthen the gut barrier, and reduce inflammation without the risks of live bacteria.
Research shows these biotics can positively influence anxiety, depression, and stress by regulating neurotransmitters, reducing inflammation, and supporting the gut-brain axis. Combining them into synbiotic formulations offers a multi-faceted approach to mental health support.
Key takeaway: Improving gut health through prebiotics, probiotics, and postbiotics can enhance mental well-being, but more clinical studies are needed to refine their use and effectiveness.
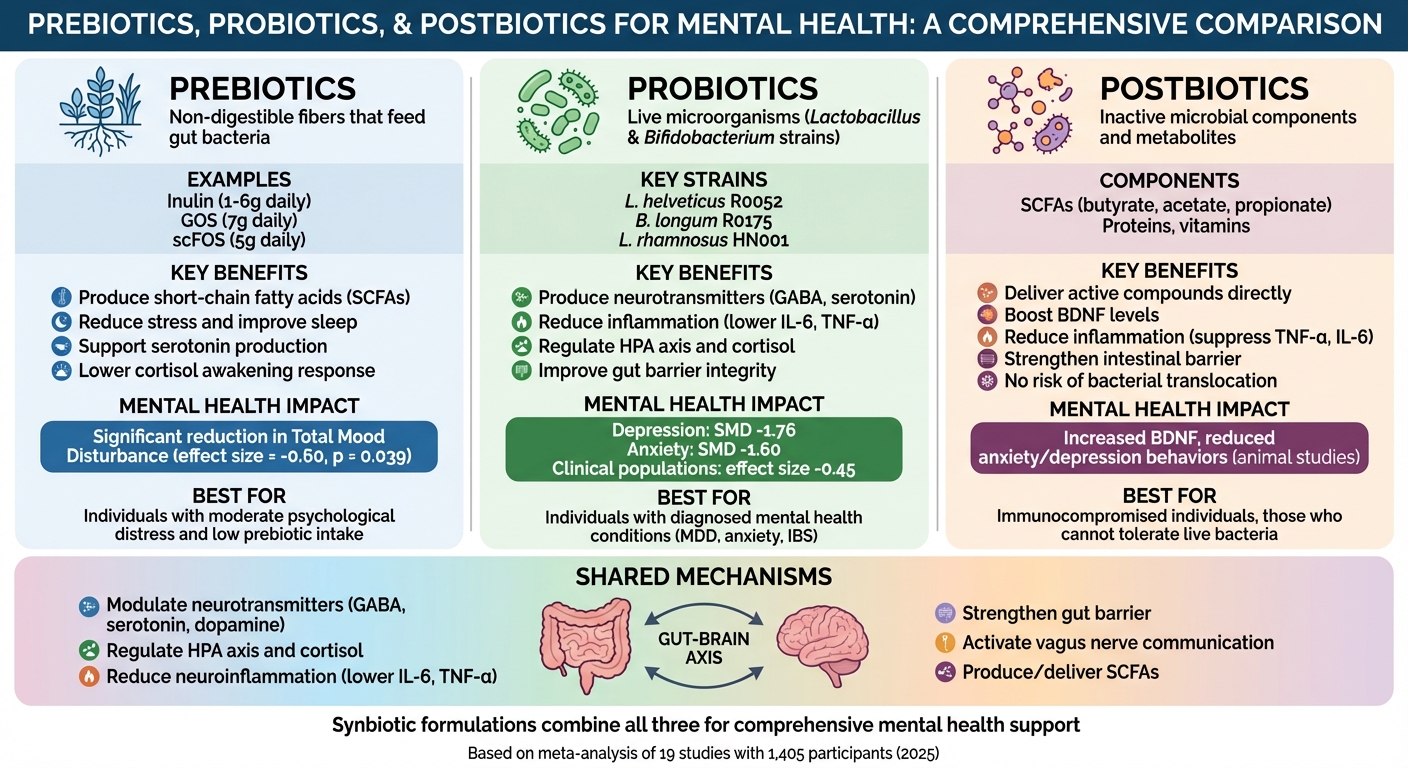
Prebiotics vs Probiotics vs Postbiotics: How They Support Mental Health
How Prebiotics Affect Mental Health
Clinical Studies on Prebiotics
The connection between prebiotics and mental health is gaining attention, with research showing both potential benefits and limitations. For instance, the "Gut Feelings" trial (2017–2019), involving 119 adults, found that a diet rich in prebiotics (seven or more servings daily) led to a significant reduction in Total Mood Disturbance (p = 0.039, effect size = -0.60) and improvements in anxiety, stress, and sleep quality [4].
However, not all findings are equally encouraging. A 2019 meta-analysis of controlled trials revealed no notable difference between prebiotics and placebo for depression (d = -0.08, p = 0.51) or anxiety (d = 0.12, p = 0.11) [6]. That said, specific groups, like individuals with irritable bowel syndrome (IBS), may see more pronounced benefits. For example, a daily dose of 5 grams of short-chain fructooligosaccharides (scFOS) reduced anxiety scores by about 2 points on the Hospital Anxiety and Depression Scale in IBS patients [7].
The effectiveness of prebiotics depends on the type and dosage. Inulin is effective at doses of 1 to 6 grams daily, while GOS (galacto-oligosaccharides) typically requires around 7 grams per day [2]. Whole-diet approaches often yield better results than supplements alone. In the "Gut Feelings" trial, participants following a high-prebiotic diet experienced significant mood improvements (p = 0.039), while probiotic supplements and synbiotics showed no significant effects compared to placebo [4].
"A high-prebiotic dietary intervention may improve mood, anxiety, stress, and sleep in adults with moderate psychological distress and low prebiotic intake." - Tanya M. Freijy et al., Researchers [4]
These findings highlight the need to delve deeper into how prebiotics influence gut bacteria and, in turn, brain function.
How Prebiotics Work in the Brain
Prebiotics don’t directly enter the bloodstream or the brain. Instead, they nourish beneficial gut bacteria like Bifidobacterium and Lactobacillus, which then produce short-chain fatty acids (SCFAs) - such as acetate, propionate, and butyrate - through fermentation [2][8].
SCFAs play a central role in the gut-brain connection. They can cross the blood-brain barrier or interact with G-protein coupled receptors (GPCRs) in the nervous system, helping to reduce inflammation and regulate neurotransmitter activity [2][3]. Prebiotics also influence tryptophan metabolism, directing it away from the depression-linked kynurenine pathway and toward serotonin production, which supports mood stability [8][7].
The HPA axis, responsible for managing stress, is another key area affected by prebiotics. A 2015 trial involving 45 healthy adults tested 5.5 grams per day of Bimuno®-galactooligosaccharide (B-GOS) over three weeks. The study, led by Schmidt et al., found that GOS reduced the cortisol awakening response and decreased attentional focus on negative information, suggesting a stress-reducing effect [8][6].
Additionally, prebiotic-driven changes in gut bacteria can boost levels of brain-derived neurotrophic factor (BDNF), a protein essential for neuron survival and the formation of new neural connections [2][3]. While these mechanisms are promising, more research is needed to understand their long-term impact.
Research Gaps and Next Steps
Despite promising findings, prebiotic research still faces challenges. Many studies have small sample sizes and short durations, typically lasting eight weeks or less [4][1]. The wide variation in prebiotic types and doses across studies also makes direct comparisons difficult.
"Prebiotics are non-viable substrates that are selectively utilised by host microorganisms and confer a health benefit." - Jerome Sarris, Western Sydney University [4]
Clinical populations seem to benefit more from biotic interventions than community samples. For example, probiotics have shown effect sizes of -0.45 in clinical groups compared to -0.09 in general populations, and this trend may extend to prebiotics as more studies are conducted [6].
Common side effects like flatulence, bloating, and abdominal discomfort can occur, especially when prebiotics are introduced in large amounts too quickly [4][5]. To minimize these effects, gradually increase prebiotic-rich foods over five days [4]. Future research should focus on long-term studies, standardized dosing, and trials targeting individuals with diagnosed mental health conditions to better identify who stands to benefit the most. Addressing these gaps will help refine how we use prebiotics to support both gut and mental health.
Probiotics for Mental Health: What the Research Shows
Psychobiotic Strains That Help Mental Health
Certain probiotic strains, often referred to as psychobiotics, have shown potential in easing symptoms of depression, anxiety, and stress. One of the most studied combinations is Lactobacillus helveticus R0052 and Bifidobacterium longum R0175, which work by regulating the HPA axis and lowering cortisol levels [7][9]. Another promising strain, Bifidobacterium longum NCC3001, has been linked to reduced amygdala activity in response to fear, benefiting individuals with irritable bowel syndrome (IBS) and depression [7][9].
Other notable strains include Lactobacillus rhamnosus HN001, which supports postpartum mood; Lactobacillus plantarum 299v, which aids cognitive function in major depressive disorder (MDD); and Bifidobacterium breve CCFM1025, which influences tryptophan metabolism [3][10]. Multi-strain formulations often provide more comprehensive benefits by targeting multiple pathways simultaneously. For example, combinations of Lactobacillus acidophilus, Lactobacillus casei, and Bifidobacterium bifidum have been used in clinical trials to address both mood disturbances and inflammation [7].
How Probiotics Work
Probiotics influence mental health through a network of gut-brain interactions. For instance, Lactobacillus and Bifidobacterium species produce GABA, a key neurotransmitter, while strains like Escherichia coli, Lactobacillus plantarum, and Streptococcus thermophilus affect serotonin production. This is significant since the majority of serotonin is synthesized in the gut [3].
The vagus nerve plays a crucial role in gut-brain communication, and studies have shown that some probiotic effects are diminished when this nerve is severed [1][3]. Probiotics also regulate the HPA axis, reducing stress-related hormones like cortisol [3][5].
In addition, probiotics can shift the balance of tryptophan metabolism, ensuring more tryptophan is available for serotonin production instead of being diverted into inflammatory pathways [3][7]. They also reduce inflammation by lowering levels of cytokines like IL-6 and TNF-α and improving gut barrier integrity, which helps prevent systemic inflammation that can disrupt neurotransmitter activity [3][7]. Neuroimaging studies, such as those using fMRI, have shown that probiotics can decrease amygdala activity and influence brain connectivity in mood-regulating networks [1][7].
Clinical Trial Results
Probiotics appear to be most effective in individuals with diagnosed mental health conditions. A 2025 meta-analysis of 19 studies involving 1,405 participants found significant reductions in depression (SMD: -1.76) and anxiety (SMD: -1.60) scores among those using probiotics, prebiotics, or synbiotics [10]. For individuals with major depressive disorder, the effect size is moderate to large (d = -0.73), while the impact on healthy populations is minimal (d = -0.09) [6].
"Probiotics yielded small but significant effects for depression (d = −.24, p < .01) and anxiety (d = −.10, p = .03)." - Richard T. Liu, Department of Psychiatry and Human Behavior, Alpert Medical School of Brown University [6]
In one randomized controlled trial involving 380 women, participants who took Lactobacillus rhamnosus HN001 from mid-pregnancy to six months postpartum saw significant reductions in depression (p = 0.037) and anxiety (p = 0.014) compared to a placebo group [7][9]. Another study with 44 IBS patients revealed that 64% of those receiving Bifidobacterium longum NCC3001 experienced a reduction in depression scores by at least two points, compared to 35% in the placebo group (p = 0.04) [7][9].
An eight-week trial involving 40 patients with major depressive disorder showed that a multi-strain probiotic reduced Beck Depression Inventory scores by 5.74 points (p = 0.001) and lowered high-sensitivity C-reactive protein levels by 1,138.7 ng/mL (p = 0.03) compared to placebo [7]. Research indicates that consistent use for two to four weeks is necessary to see benefits, with longer trials (over one month) yielding better outcomes (d = -0.28) than shorter ones (d = -0.10) [6][9][11]. These findings highlight the potential of probiotics as a targeted approach to improving mental health.
Postbiotics and Mental Health: New Research
Understanding Postbiotics
Postbiotics are essentially preparations of inactivated microorganisms and their components that can promote health. According to the International Scientific Association for Probiotics and Prebiotics (ISAPP), they are defined as "a preparation of inanimate microorganisms and/or their components that confers a health benefit on the host" [3][5]. Unlike probiotics, which rely on live bacteria, postbiotics include inactive microbial cells, fragments like pili, and metabolic by-products.
These preparations provide functional components like short-chain fatty acids (SCFAs) such as butyrate, acetate, and propionate, along with proteins, vitamins, and other metabolites produced during gut bacterial fermentation [3][5]. Notably, SCFAs like butyrate can either signal through the vagus nerve or cross the blood-brain barrier, influencing brain activity [3]. Postbiotics also play a role in regulating neuroactive compounds like GABA, serotonin, and dopamine, which are critical for maintaining mental health [3][2]. These features make postbiotics a fascinating area of research in understanding their impact on mental well-being.
How Postbiotics Influence Mental Health
Unlike prebiotics, which require fermentation to generate beneficial compounds, postbiotics deliver these active components directly. This direct action allows them to impact mental health through several mechanisms. For instance, postbiotics have been shown to boost levels of Brain-Derived Neurotrophic Factor (BDNF), a protein vital for the survival of neurons and the growth of new brain cells [3]. A 2021 study on heat-killed Lactobacillus paracasei PS23 in adolescent male mice with corticosterone-induced depression demonstrated that 40 days of treatment (10^8 CFU/0.2 mL per day) increased BDNF levels. This treatment also enhanced mineralocorticoid and glucocorticoid receptor activity, resulting in reduced anxiety- and depression-like behaviors [3].
Postbiotics also help reduce inflammation by suppressing pro-inflammatory cytokines like TNF-α and IL-6. SCFAs, in particular, interact with G-protein coupled receptors in the central nervous system, helping to regulate inflammation associated with mental health disorders [2][3]. Butyrate, for example, has shown antidepressant effects by inhibiting histone deacetylase, which promotes histone hyperacetylation. Additionally, these metabolites strengthen the intestinal barrier, potentially preventing systemic inflammation that could disrupt neurotransmitter activity. When used alongside prebiotics and probiotics, postbiotics contribute to a comprehensive approach to modulating the gut-brain axis.
Another advantage of postbiotics is their safety. Since they don't contain live bacteria, they eliminate the risk of bacterial translocation or systemic infection, particularly in vulnerable populations like immunocompromised individuals or those with cardiac valvular disorders [5]. Their stability and long shelf life make them even more practical for use [3][5].
Current Studies and Limitations
While the mechanisms of postbiotics show promise, research into their effects on mental health is still in its early stages. Most findings come from animal studies, which have shown encouraging results in reducing anxiety- and depression-like behaviors. However, clinical trials involving humans are currently lacking [5]. As of late 2021, no interventional studies had been conducted to evaluate the role of postbiotics in mental health or neurocognitive disorders.
"Postbiotics and paraprobiotics have the potential to be used as pharmacological agents in the prevention and treatment of various psychiatric and neurocognitive disorders." - Kannayiram Alagiakrishnan, Division of Geriatric Medicine, University of Alberta [5]
Although mechanistic studies highlight the potential benefits of postbiotics, more randomized controlled trials are needed. These studies would help confirm the effects observed in preclinical research and establish the most effective dosages, treatment durations, and formulations for specific mental health conditions.
sbb-itb-1bbfe7f
Using Biotics Together for Mental Health
Common Pathways Across All Biotics
Prebiotics, probiotics, and postbiotics all influence mental health through shared mechanisms. One key way they work is by modulating neurotransmitters like GABA, serotonin, dopamine, and noradrenaline - chemicals that play a major role in mood and cognitive function. They also help regulate the HPA axis, which manages your body's stress response by controlling hormones like cortisol and corticosterone.
Another important function is reducing inflammation. These biotics lower pro-inflammatory cytokines (like IL-6 and TNF-α) while increasing anti-inflammatory IL-10. They also strengthen the intestinal barrier, preventing "leaky gut", which can allow harmful endotoxins to enter the bloodstream and trigger neuroinflammation. On top of that, they influence the vagus nerve, a critical communication pathway between the gut and brain that impacts neurochemical levels in the central nervous system [2][3].
One of the most vital shared mechanisms is the production of short-chain fatty acids (SCFAs). Prebiotics fuel probiotics, which then produce SCFAs like butyrate, acetate, and propionate. These molecules can cross the blood-brain barrier or activate GPCRs, helping to regulate inflammation and metabolism [2][3]. This interconnected process highlights why using biotics together can provide more robust mental health support than relying on one alone. These shared pathways underline the potential of combining biotics, as explored below.
3-in-1 Synbiotic Formulations
Combining prebiotics, probiotics, and postbiotics into a single product creates a synergistic effect. Prebiotics act as fuel for probiotics, ensuring the gut-brain axis functions properly. Together, they enhance both immune and nervous system health more effectively than when used individually [2].
"The combined use of pro-and prebiotics, called synbiotics, has a synergistic effect and plays an important role in controlling and reducing the risk of some diseases, including mental disorders." - Ansari et al., Frontiers in Nutrition [2]
Three-in-one synbiotic formulations target multiple mental health pathways at once. For example, Begin Rebirth RE-1™ (https://beginrebirth.com) combines prebiotics (4.5g of GOS and inulin), probiotics (500 billion CFU of Human Origin Strains), and postbiotics, all delivered via a proprietary Lyosublime™ system that doesn’t require refrigeration.
Postbiotics in these formulations are especially noted for their safety profile. Since they don’t contain live bacteria, they eliminate risks like bacterial translocation or systemic infections - making them a safer option for immunocompromised individuals or those with conditions like heart disease [5].
Areas for Future Research
While the shared pathways and benefits of synbiotics are promising, more research is needed to refine their use. For example, while high-prebiotic diets have been shown to improve mood, the additional benefits of combining prebiotics with probiotics and postbiotics remain unclear [4][12].
Future studies should focus on long-term randomized controlled trials in humans, especially for postbiotics, where most evidence currently comes from animal research. Critical areas to explore include determining the most effective dosages, treatment durations, and formulations for specific mental health conditions. Biomarker analysis could help identify which individuals respond best to different biotic combinations, paving the way for personalized mental health treatments. Additionally, research should examine how specific probiotic strains pair with particular prebiotic fibers and how postbiotic metabolites can be standardized to ensure consistent therapeutic effects.
How to Fix Your Brain-Gut Connection: Anxiety and the Brain-Gut Microbiome Axis
Conclusion
Research shows that prebiotics, probiotics, and postbiotics work together to support mental health by influencing the gut-brain axis through various pathways. They help regulate neurotransmitters, manage stress hormones like cortisol by balancing the HPA axis, and reduce neuroinflammation by lowering pro-inflammatory cytokines such as IL-6 and TNF-α [2][13][7]. With over 1 billion people worldwide affected by mental health disorders and around 4.4% of the global population living with depressive disorders [2], these biotic interventions offer a promising addition to traditional treatments.
When considering these interventions, an evidence-based approach is critical. Research highlights that specific psychobiotic strains, particularly from Lactobacillus and Bifidobacterium, have consistently shown positive effects on mental health [2][13]. A 2023 review of nine clinical trials found that eight demonstrated significant improvements in symptoms of depression and anxiety when using probiotics or prebiotics [7]. However, challenges like small sample sizes and inconsistent methodologies remain, emphasizing the need for more rigorous clinical trials to confirm their therapeutic potential [2][1].
Combining biotics - especially in 3-in-1 synbiotic formulations - offers a comprehensive approach by addressing multiple mental health pathways at once. Prebiotics fuel probiotics to produce beneficial SCFAs, while postbiotics provide a safer option for those who may not tolerate live bacteria [2][5][13]. Products like Begin Rebirth RE-1™ illustrate this strategy, combining 4.5 g of prebiotics (GOS and inulin), 500 billion CFU of Human Origin Strains, and postbiotics delivered through a proprietary Lyosublime™ system.
Looking ahead, more long-term randomized controlled trials are essential to determine the best dosages, treatment durations, and strain-specific effects for different mental health conditions. Future research should also focus on individual responses to these biotics, paving the way for more personalized mental health solutions.
FAQs
How do prebiotics, probiotics, and postbiotics support mental health?
Prebiotics, probiotics, and postbiotics work together to maintain a healthy gut-brain connection, which plays a crucial role in mental health. Prebiotics are fibers that nourish beneficial gut bacteria, encouraging them to produce compounds like short-chain fatty acids (SCFAs). These compounds help strengthen the gut lining and reduce inflammation. Probiotics are live bacteria that populate the gut, competing with harmful microbes and producing neurotransmitters like serotonin and GABA, both of which are key players in mood regulation. Postbiotics are the bioactive by-products of these bacteria, including SCFAs and microbial-derived neurotransmitters, which help manage inflammation and communicate with the brain through the vagus nerve.
Together, these three components work in harmony: prebiotics feed probiotics, probiotics create postbiotics, and postbiotics send signals that impact mood and cognitive function. Products like Begin Rebirth RE-1™ combine all three elements into a science-backed formula aimed at resetting the microbiome, supporting neurotransmitter balance, and promoting mental wellness.
How do prebiotics support mental health?
Prebiotics are essential for promoting mental well-being, largely because they support the vital gut-brain connection. They’ve been shown to help ease feelings of depression and anxiety, improve how we handle stress, and even uplift overall mood. On top of that, prebiotics might play a role in improving sleep quality and contributing to a stronger sense of overall wellness.
How does this work? Prebiotics feed the beneficial bacteria in your gut, which helps maintain a healthy balance of neurotransmitters - key players in mental health. Adding prebiotics to your daily routine could be a straightforward yet impactful way to nurture both your gut and your mind.
Are postbiotics safe to use for mental health support?
Postbiotics are generally safe and well-tolerated for most healthy adults. Since they consist of non-living bacterial components - like short-chain fatty acids or microbial metabolites - the risk of infection is extremely low. That said, some people may experience mild digestive symptoms, such as gas or bloating, particularly when taking higher doses or if they have a sensitive digestive system.
In rare cases, there’s a chance of allergic reactions to specific ingredients or complications from product contamination during manufacturing. To avoid any issues, it’s a good idea to start with a low dose and pay attention to how your body reacts.
Begin Rebirth RE-1™ offers a clinically-supported blend of prebiotics, probiotics, and postbiotics. This formula is designed to reset your gut microbiome while helping reduce the chances of mild gastrointestinal discomfort.