Stress impacts more than just your mind - it disrupts your gut health too. Here's what you need to know:
- Your gut microbiome is home to trillions of microorganisms that influence digestion, immunity, and even your brain through the gut-brain axis.
- Stress triggers changes in gut bacteria, weakens the gut lining (leading to "leaky gut"), and increases inflammation, which can worsen mental health.
- Adaptogens, like Ashwagandha and Rhodiola, are plant-based compounds that help regulate stress hormones (like cortisol) and support gut health.
- Combining adaptogens with synbiotics (probiotics + prebiotics) can restore gut balance, reduce inflammation, and improve resilience to stress.
Scientific studies reveal that stress accounts for about 5% of gut microbiota variation - on par with diet and genetics. Addressing stress-related gut imbalances with a dual approach (adaptogens + synbiotics) offers a practical way to support mental and physical health.
Let’s dive deeper into how stress disrupts your gut and how these natural solutions can help.
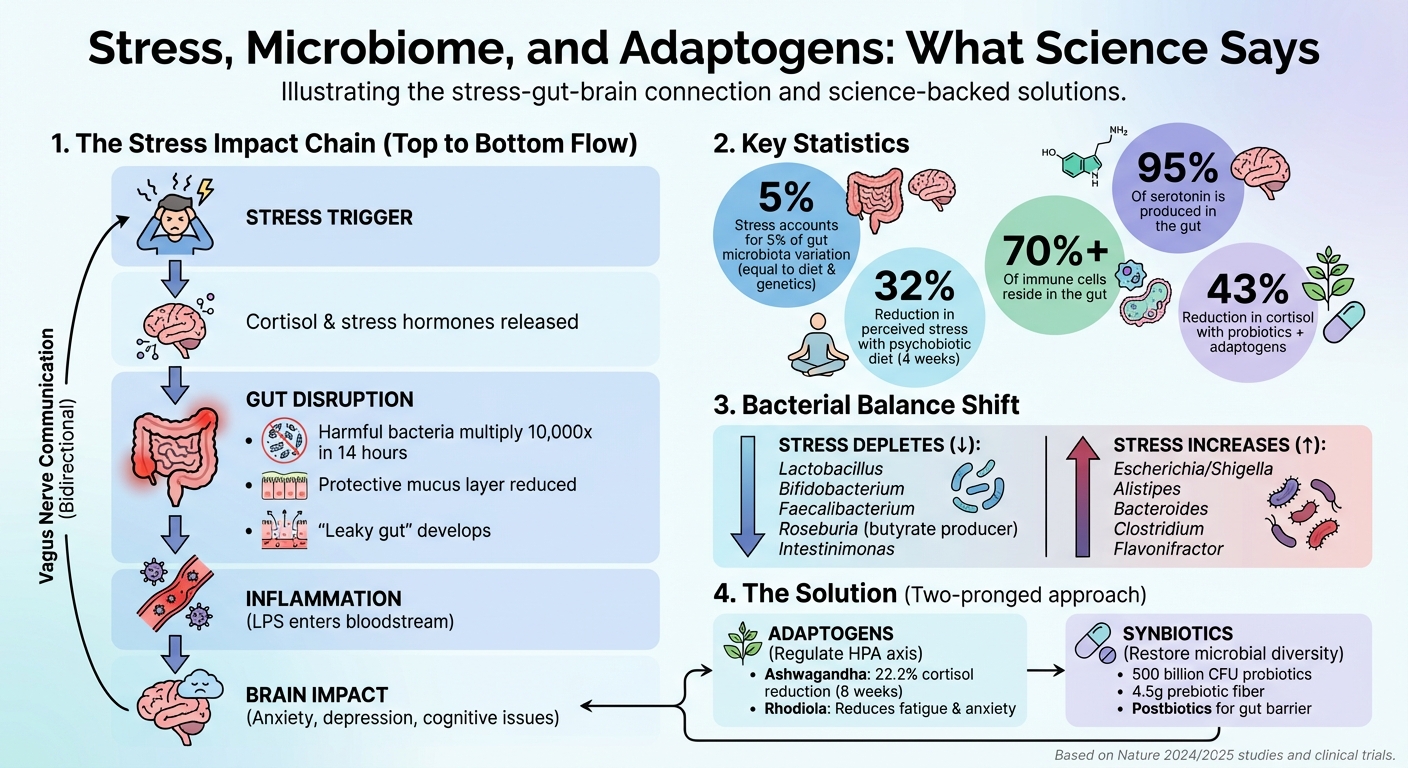
How Stress Disrupts the Gut-Brain Axis: A Visual Guide
How Stress Disrupts the Gut Microbiome
How Stress Changes the Microbiome
When you're stressed, your body releases hormones like cortisol, norepinephrine, and epinephrine. These hormones don't just affect your mood - they also impact the bacteria in your gut. For example, catecholamines can cause harmful gram-negative bacteria to multiply rapidly, increasing their numbers by up to 10,000 times in just 14 hours [8][10].
Stress also damages the gut's defenses. It reduces the protective mucus layer and weakens tight junction proteins, which are crucial for keeping the gut lining intact. This damage leads to a condition often called "leaky gut", where harmful substances like lipopolysaccharides (LPS) and pathogenic bacteria can pass into the bloodstream. Once in the bloodstream, these substances can trigger inflammation [8][10].
Chronic stress further disrupts the balance of gut bacteria, increasing the ratio of Bacteroidetes to Firmicutes. This shift favors pro-inflammatory bacteria over beneficial ones. Elevated cortisol levels are also linked to reduced populations of helpful bacteria, such as Ruminococcus species [8]. These changes in the gut microbiome set the stage for understanding the gut-brain connection and the potential role of adaptogens in mitigating stress effects.
Research Study Findings
Scientific research backs up these observations with hard data. A dual-study report in Nature (2024/2025) explored the gut microbiomes of two groups of healthy adults (Study 1: n=62; Study 2: n=74). The findings revealed that stressful life events accounted for 5% of the variance in gut microbiota composition - a level of influence similar to that of host genetics, which explained 1.9% to 8.1% [3]. As the authors noted:
"Stressful life events may have comparable importance on the composition of the gut microbiome as diet or genetics." [3]
In the second study, which focused on women with an average age of 41.6 years, researchers found a significant link between perceived stress and the presence of harmful pathogens like Escherichia/Shigella (r=0.26, p=0.02) [3]. At the same time, beneficial bacteria such as Intestinimonas and Roseburia - key producers of the anti-inflammatory compound butyrate - were either absent or undetectable in participants experiencing high levels of stress [3].
Stress not only reduces the diversity of gut bacteria (both alpha and beta diversity) but also weakens the overall resilience of the gut ecosystem [8][3]. This imbalance allows harmful bacteria like Alistipes, Bacteroides, Eggerthella, Clostridium, and Flavonifractor to thrive while depleting beneficial strains such as Lactobacillus, Bifidobacterium, Faecalibacterium, Blautia, Coprococcus, and Akkermansia [8][3][9]. These shifts not only promote inflammation and compromise the gut barrier but can also negatively affect memory and emotional regulation.
The Gut-Brain Axis: How the Microbiome Affects Stress
Gut Bacteria and Emotional Regulation
Your gut bacteria play a major role in shaping how your brain handles stress. They communicate with the brain through neural, hormonal, and immune pathways, creating a dynamic connection known as the gut-brain axis [2].
Research has shown that gut bacteria are essential for a balanced stress response. For example, studies on germ-free animals - those raised without any gut bacteria - reveal an exaggerated stress response marked by elevated levels of ACTH and corticosterone [1]. Interestingly, introducing specific bacteria like Bifidobacterium infantis into these animals can normalize their stress responses [2].
The vagus nerve, a key communication highway between the gut and brain, is central to this process. In one study, the probiotic strain Lactobacillus rhamnosus (JB-1) reduced anxiety-like behavior caused by stress - but only when the vagus nerve was intact [2]. As Jane A. Foster from McMaster University's Department of Psychiatry & Behavioural Neurosciences explains:
"The vagus nerve has been proposed to serve as the most important neural pathway for bidirectional communication between gut microbes and the brain." [2]
Gut microbes also influence the production of neurotransmitters, the brain's chemical messengers. Did you know that about 95% of serotonin, a critical mood regulator, is produced in the gut [2]? Beyond serotonin, gut bacteria help regulate other neurotransmitters like GABA, dopamine, and noradrenaline [2]. They even produce short-chain fatty acids (SCFAs) like butyrate, which can cross the blood-brain barrier or signal through the vagus nerve to reduce neuroinflammation and boost stress resilience [3]. These combined actions show how gut bacteria contribute to both mood regulation and the ability to handle stress.
The microbiome even impacts the physical structure of stress-related brain regions. Germ-free animals, for instance, show increased growth in the amygdala (the brain's fear center) and abnormal neurogenesis in the hippocampus, which is essential for memory and emotional regulation [2].
Immune System and Inflammation Connections
Stress doesn't just affect your mind - it can disrupt the gut lining, allowing harmful substances like LPS (lipopolysaccharides) to enter your bloodstream and trigger widespread inflammation [8]. This is a big deal because the gut is home to over 70% of your immune cells [8]. Once these inflammatory signals reach the brain, they activate microglia - immune cells in the brain - which release pro-inflammatory cytokines such as IL-1β, IL-6, and TNFα [8]. Over time, this chronic inflammation has been linked to mental health conditions like depression and anxiety [1].
The composition of your gut microbiota also plays a role in this inflammatory process. Some bacteria, like segmented filamentous bacterium, encourage the development of Th17 immune cells, which have been associated with depressive-like behaviors [8]. A 2024 study found that higher levels of Clostridium were negatively linked to biological stress resilience, as measured by heart rate variability (r = -0.37, p = 0.003) [3]. On the flip side, people who are more resilient to stress often have higher levels of SCFA-producing bacteria, which help maintain the gut barrier and reduce inflammation [4]. For example, butyrate, produced by bacteria like Roseburia, is essential for keeping the intestinal wall intact by supporting tight junctions [3].
This intricate relationship between the gut, immune system, and brain highlights how maintaining a balanced microbiome can influence both mental and physical health. It also opens the door to exploring how natural compounds like adaptogens might help restore this balance.
Why Fixing Your Gut Could Help Your Depression!
sbb-itb-1bbfe7f
Adaptogens and Their Effects on Stress and Gut Health
Adaptogens offer a powerful twofold approach to tackling stress and supporting gut health. They not only help the body manage stress but also address the gut imbalances that stress can cause.
What Are Adaptogens?
Adaptogens are natural plant compounds known for their ability to help the body resist stress and maintain balance [5][7]. These compounds don't just ease the stress response - they actively work to counteract the disruptions stress can create in the gut.
The term "adaptogen" was first introduced to describe substances that enhance the body’s ability to resist stress in a general, non-specific way. This resistance is closely tied to the neuroendocrine-immune system, which plays a key role in how our bodies handle stress [5]. As Alexander Panossian of the Swedish Herbal Institute Research & Development explains:
"Adaptogens work like a stress vaccine (stress-mimetic) by activating stress-induced self-defense mechanisms in order to adapt the cell and organism to mitigate stress-induced harmful effects." [5]
The key to their effectiveness lies in how they regulate the hypothalamic-pituitary-adrenal (HPA) axis, the system responsible for managing stress. Adaptogens influence stress mediators like cortisol, nitric oxide, and proteins such as Heat Shock Protein 70 (Hsp70) [5][6]. By interacting with glucocorticoid receptors, they help bring chronically high cortisol levels back to normal and restore balance to the HPA axis [12]. This mechanism ties directly into the gut-brain connection, making adaptogens a valuable tool for stress recovery when paired with synbiotics.
Scientific Evidence for Adaptogens and Gut Health
Studies back up the benefits of adaptogens in reducing stress and improving gut health. For example, an 8-week randomized controlled trial found that Ashwagandha (Withania somnifera) lowered serum cortisol levels by 16.05% after four weeks and by 22.2% after eight weeks. A meta-analysis through June 2023 further supported these findings, showing an average decrease of -3.27 ug/dL in cortisol levels among stressed adults [6][12].
Rhodiola (Rhodiola rosea) has shown similar benefits, reducing fatigue and anxiety while helping to regulate cortisol levels [6][7]. Its active component, rosiridin, also inhibits MAO-A/B enzymes, which helps maintain neurotransmitter balance and supports emotional well-being [5][7]. Other adaptogens, like Asian Ginseng (Panax ginseng) and Eleuthero (E. senticosus), are known to combat fatigue and influence immune system regulation [7].
These findings highlight the potential of adaptogens to address both stress and its effects on gut health, offering a holistic way to support overall well-being.
Combining Adaptogens and Synbiotics for Stress Recovery
When it comes to tackling stress, combining adaptogens and synbiotics can offer a more effective solution than either strategy alone. Stress often disrupts both the HPA axis and the gut microbiome, and addressing just one of these areas may not be enough. By combining adaptogens with synbiotics, you create a dual-action approach that works on both ends of the gut-brain axis - helping to regulate cortisol levels while rebalancing gut bacteria and reducing inflammation [6][13].
The Science Behind Synbiotics
Synbiotics, which pair probiotics with prebiotics, go beyond what either component can achieve on its own. They work together to restore gut diversity and reduce inflammatory gene expression more effectively than either probiotics or prebiotics used individually [13].
Here’s how it works: prebiotics fuel the growth of beneficial bacteria already in your gut, probiotics introduce live microorganisms, and the fermentation process produces postbiotics - bioactive compounds like short-chain fatty acids. These postbiotics help reduce systemic inflammation and strengthen the gut barrier [14]. This three-step process tackles the root causes of stress-related gut issues rather than just masking the symptoms.
In a study published in Frontiers in Immunology in June 2021, researchers from the Icahn School of Medicine at Mount Sinai demonstrated how this synergy works. Dr. Giulio Maria Pasinetti’s team tested a synbiotic that combined Lactobacillus plantarum ATCC 793, Bifidobacterium longum ATCC 15707, and a grape-derived polyphenol prebiotic on mice exposed to chronic stress. The results were impressive: the synbiotic reduced inflammatory genes (Ccl2, Ccl5, Icam) in the brain and restored gut diversity - outcomes that neither the probiotics nor the prebiotics achieved on their own [13][11].
These findings aren’t just limited to lab studies. In real-world scenarios, a psychobiotic diet rich in prebiotics and fermented foods led to a 32% reduction in perceived stress after just four weeks [15]. When combined with multi-strain probiotics, studies on academic stress showed even more dramatic results: a 43.02% reduction in serum cortisol and a 38.62% decrease in perceived stress [6].
Begin Rebirth RE-1™: A Rapid Microbiome Reset
Begin Rebirth RE-1™ takes this science and puts it into action with a 3-in-1 eubiotic formula designed to quickly restore gut health. Each sachet delivers 500 billion CFU of Human Origin Strains (HOSt™) - probiotics specifically designed to survive the digestive process and reach the gut intact. It also includes 4.5g of prebiotic fiber (a mix of GOS and inulin) to nourish beneficial bacteria, as well as postbiotics to support gut barrier integrity right away.
Thanks to the Lyosublime™ delivery system, the formula is easy to use and doesn’t require refrigeration, making it convenient for daily use. Whether you follow a 7-day, 4-week, or 12-week protocol, this high-potency synbiotic formula provides targeted support for stress-related gut imbalances. It works on the same inflammatory pathways and microbial issues identified in clinical studies [13][11].
When paired with adaptogens like Ashwagandha or Rhodiola, Begin Rebirth RE-1™ offers a comprehensive approach to stress recovery. It helps regulate cortisol levels while restoring microbial balance, creating a powerful framework for addressing stress from multiple angles. This combination lays the groundwork for a deeper dive into holistic stress management strategies.
Conclusion
When stress activates the HPA axis, it triggers cortisol release, which disrupts gut health by reducing microbial diversity. This process depletes essential butyrate-producing bacteria and weakens the intestinal barrier. As a result, harmful inflammatory compounds enter the bloodstream, affecting brain function and increasing the risk of anxiety, depression, and even neurodegenerative disorders.
Addressing this issue requires a two-pronged strategy: supporting both the gut and the body's stress response. Adaptogens help regulate cortisol levels, while synbiotics work to restore gut microbial balance and strengthen the intestinal barrier. Research shows that combining these approaches offers a more effective way to counteract the complex effects of chronic stress.
One example of this dual approach in action is Begin Rebirth RE-1™, a 3-in-1 synbiotic solution. It delivers 500 billion CFU, 4.5 g of prebiotic fiber, and postbiotics designed to correct stress-induced imbalances in the gut. Whether you're grappling with chronic stress, a disrupted gut microbiome, or both, this clinically supported synbiotic targets the inflammatory pathways and microbial disruptions tied to stress. It represents a practical, research-driven method for stress recovery.
The link between stress, gut health, and mental well-being isn't just a theory - it's a well-documented reality supported by decades of research. With over 20% of adults in the United States experiencing mental health challenges connected to disruptions in the microbiota–gut–immune–brain axis [16], finding effective solutions is more critical than ever. By integrating adaptogens with cutting-edge synbiotic technology, you can take proactive steps to manage stress and restore balance to the gut-brain connection.
FAQs
How do adaptogens help manage stress-related gut imbalances?
Adaptogens are plant-based compounds that help the body manage stress by balancing hormonal and cellular responses. When stress strikes, it often triggers the release of cortisol - a hormone that, in excess, can damage the gut barrier. This damage may lead to an imbalance in the gut's microbiome, a condition known as dysbiosis. Adaptogens work to counteract these effects by lowering cortisol levels, shielding gut cells from inflammation and oxidative stress, and maintaining the strength of the gut lining.
Many adaptogens also encourage the growth of beneficial gut bacteria like Lactobacillus and Bifidobacterium, which are crucial for a thriving microbiome. By addressing stress-induced disruptions, adaptogens can enhance gut health, reduce inflammation, and support a more balanced microbiome. Consistent use of adaptogenic blends has been linked to improved digestion, less intestinal discomfort, and overall better gut health.
How do synbiotics help restore gut health during stress?
Synbiotics, which blend probiotics with prebiotics that feed them, play an important role in restoring gut health disrupted by stress. When stress throws the gut microbiome off balance, it can lead to inflammation, immune system issues, and even mood shifts. Synbiotics help by replenishing beneficial bacteria and supplying the nutrients they need to thrive, promoting a balanced and diverse microbial environment.
Studies indicate that synbiotics not only enhance gut health but also strengthen the gut-brain connection, easing stress-related issues like anxiety and digestive discomfort. By stabilizing the gut-brain axis, they support immune function, reduce inflammation, and build resilience to stress. For instance, Begin Rebirth RE-1™, a clinically-supported 3-in-1 eubiotic synbiotic, provides 500 billion CFU per serving along with targeted prebiotics. It’s designed to reset the microbiome in as little as seven days, helping restore gut balance and overall well-being during stressful periods.
Can stress-related changes in the gut microbiome impact mental health?
Stress has a powerful impact on the gut microbiome, which can, in turn, influence mental health. Research indicates that both short-term and long-term stress can decrease beneficial gut bacteria, such as Lactobacillus and Bifidobacterium. At the same time, it can encourage the growth of harmful bacteria and lead to increased intestinal permeability - commonly referred to as a "leaky gut." This condition can trigger inflammation, disrupt the communication between the brain and gut, and potentially influence mood and how the body handles stress.
Additionally, studies have found a connection between elevated stress levels and reduced gut microbial diversity, which has been linked to symptoms of anxiety and depression. Since adaptogens are known for aiding the body in managing stress, products that combine prebiotics, probiotics, and postbiotics - like Begin Rebirth RE-1™ - may help rebalance the gut and promote better mental health.