Prebiotics - plant-based fibers that nourish gut bacteria - may hold the key to improving PTSD recovery. Research shows the gut-brain axis, a communication network between the gut and brain, plays a role in mental health. Trauma can disrupt gut health, leading to inflammation and worsening PTSD symptoms. By restoring gut balance, prebiotics support the production of short-chain fatty acids (SCFAs), which reduce inflammation and improve emotional regulation.
Key Insights:
- PTSD and Gut Health: Trauma weakens the gut lining, allowing toxins to trigger brain inflammation.
- SCFAs: Produced by beneficial gut bacteria, they protect the brain and reduce stress-related inflammation.
- Clinical Evidence: Studies show prebiotics combined with therapy can improve PTSD symptoms by enhancing gut-brain communication.
To support recovery, incorporate prebiotic-rich foods like garlic, onions, and bananas, or consider supplements. Pairing prebiotics with therapy creates a more effective recovery plan.
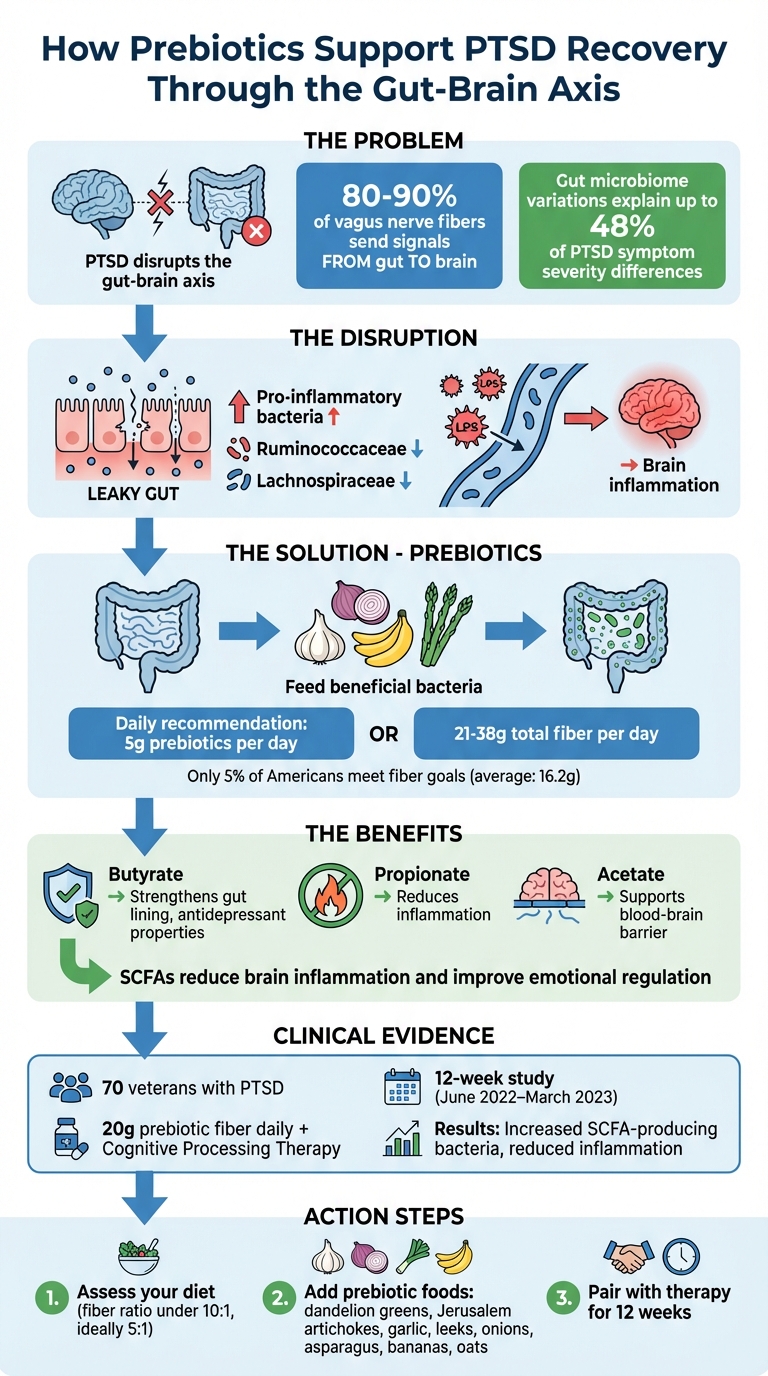
How Prebiotics Support PTSD Recovery Through the Gut-Brain Axis
Stress, Trauma, and Dysbiosis: Connecting the Gut-Brain Axis to Autoimmune Disease
The Gut-Brain Axis and PTSD
The gut-brain axis is essentially a two-way communication system between your digestive system and your central nervous system. This intricate connection works through four main pathways: the vagus nerve (neural), the HPA axis (endocrine), immune signaling, and metabolic processes [1][8]. Interestingly, 80–90% of the vagus nerve fibers send sensory information from the gut to the brain, rather than the other way around [8]. In simpler terms, your gut is constantly sending signals that shape how your brain handles stress and emotions. However, when trauma disrupts gut health, this communication can break down.
In cases of PTSD, this system is thrown off balance. The intestinal barrier in your gut weakens - often referred to as "leaky gut" - allowing bacterial toxins like lipopolysaccharides (LPS) to escape into your bloodstream [2][7]. These toxins can cross into the brain, sparking inflammation in areas responsible for fear and emotional regulation. What happens next is a harmful cycle: trauma damages gut health, and poor gut health worsens PTSD symptoms, creating a feedback loop that’s hard to escape.
How Gut Imbalances Impact Mental Health
Studies have found that PTSD is associated with an increase in pro-inflammatory bacteria and a decrease in beneficial strains such as Ruminococcaceae and Lachnospiraceae [2][4]. These harmful bacteria release toxins and inflammatory compounds that disrupt your body's ability to produce neurotransmitters - the brain’s chemical messengers that regulate mood and stress.
The effects are striking. Research has shown that variations in the gut microbiome can explain up to 48% of the differences in PTSD symptom severity among individuals [4]. Inflammatory cytokines from these harmful bacteria can travel to the brain, interfering with processes like fear-extinction learning, which is crucial for recovering from traumatic memories [1][2]. On the flip side, beneficial bacteria produce short-chain fatty acids (SCFAs) that help reduce inflammation and strengthen the blood-brain barrier, offering some protection against these disruptions.
Short-Chain Fatty Acids and Their Role in Brain Health
Beneficial gut bacteria create short-chain fatty acids (SCFAs) by fermenting dietary fiber. The three main SCFAs - butyrate, propionate, and acetate - serve as powerful molecules that lower brain inflammation and help maintain the integrity of the blood-brain barrier [2][3]. For example, butyrate has antidepressant properties and strengthens the gut lining by acting as a histone deacetylase inhibitor [5].
In January 2025, Dr. Robin M. Voigt and her team at the Rush Center for Integrated Microbiome and Chronobiology Research conducted a 12-week pilot study involving 70 veterans with PTSD. They paired Cognitive Processing Therapy with a prebiotic fiber blend containing resistant starch, inulin, and rice bran. The results revealed that PTSD severity was closely tied to a reduced presence of bacteria that produce propionate [5]. This suggests that a lack of SCFA-producing bacteria deprives the brain of essential tools to combat inflammation and manage stress. The study highlights how targeted prebiotic supplementation could complement traditional PTSD therapies by supporting SCFA production, which is key to restoring the gut-brain connection in PTSD recovery.
Research on Prebiotics for PTSD Recovery
Clinical Studies on Prebiotics and PTSD
From June 2022 to March 2023, the Rush Center for Integrated Microbiome and Chronobiology Research conducted a 12-week, double-blind, placebo-controlled trial under the leadership of Dr. Robin M. Voigt. This study focused on 70 veterans with PTSD, all undergoing an Intensive Treatment Program at the Road Home Program in Chicago. Participants were given either a placebo or a prebiotic blend (20 g of fiber daily through two bars) alongside therapy sessions. The results, published in January 2025, revealed some fascinating insights: the prebiotic intervention not only altered the intestinal microbiota but also increased stool short-chain fatty acid (SCFA) levels.
One particularly noteworthy finding was the link between PTSD severity and reduced levels of bacteria that produce propionate. Clinical assessments using the PTSD Checklist for DSM-5 (PCL-5) showed meaningful symptom improvement in specific subsets of participants. These results offer a new perspective on how prebiotic-induced increases in SCFAs may help combat inflammation.
"This study suggests that targeting the intestinal microbiome through prebiotic supplementation could represent a promising avenue for enhancing treatment outcomes in some individuals with PTSD."
- Robin M. Voigt, PhD, Rush University Medical Center [5]
Prebiotics, Inflammation, and the Gut-Brain Connection
Expanding on these clinical findings, prebiotics appear to play a key role in addressing systemic inflammation associated with PTSD. Through the gut-brain axis, changes in gut bacteria can directly influence inflammation and PTSD symptoms. Research has shown that PTSD is often linked to a pro-inflammatory gut microbiome, which tends to have higher levels of harmful Gram-negative bacteria and fewer beneficial metabolites.
Prebiotics help by boosting SCFA levels, which in turn strengthen the intestinal barrier and prevent lipopolysaccharides (LPS) from leaking into the bloodstream. This leakage is a known trigger for inflammatory responses. Beyond this, SCFAs act as signaling molecules, influencing the gut-brain axis by interacting with pathways like the vagus nerve, the hypothalamic-pituitary-adrenal axis, and neurotransmitter production. These mechanisms complement psychological therapies such as Cognitive Processing Therapy, offering a more holistic approach to PTSD treatment [5].
sbb-itb-1bbfe7f
Adding Prebiotics to Your PTSD Recovery Plan
Step 1: Take a Closer Look at Your Diet
Start by evaluating how much fiber you’re getting each day. On average, Americans consume about 16.2 grams of fiber daily, which falls short of the recommended 21–38 grams, depending on factors like age and sex. In fact, only 5% of people meet this daily goal [13]. Since prebiotics are found in fiber-rich foods, it’s likely that many are missing out on these gut-supporting nutrients.
A quick way to identify high-fiber foods is by checking the carbohydrate-to-fiber ratio on nutrition labels. Aim for foods with a ratio under 10:1 - ideally closer to 5:1 [13]. For prebiotics specifically, the International Scientific Association for Probiotics and Prebiotics suggests consuming 5 grams per day [10]. As an example, just half a small (4-ounce) onion provides this amount [10].
"Nutrition is the main therapeutic tool to positively influence the microbiome. A diet rich in fiber, vegetables, and fruit helps establish a varied and rich microbiome that promotes the health of the host."
- David Rakel, MD, and David Lessens, MD, MPH [13]
Use this information to adjust your diet and incorporate foods or supplements that target prebiotic intake.
Step 2: Add Prebiotic Foods and Supplements to Your Routine
Focus on foods that contain prebiotic fibers known to support PTSD recovery, such as inulin, resistant starch (type 2), resistant maltodextrin, and rice bran [5]. Some of the best sources include dandelion greens, Jerusalem artichokes, garlic, leeks, and onions [10]. Other great options are asparagus, bananas, oats, barley, legumes, and whole grains [9][11][12].
The Mediterranean diet is also a strong choice. Its emphasis on vegetables, fruits, legumes, and fish has been shown to promote beneficial gut bacteria like Eubacterium eligens, which is linked to reduced PTSD symptoms [6]. On the flip side, try to limit red and processed meats, as they’ve been associated with increased PTSD symptoms and fewer helpful gut bacteria [6].
When introducing prebiotics, start small - about a quarter of a typical serving - to minimize side effects like gas or bloating. Gradually increase your portions over time [9][11]. If you prefer supplements, look for options containing GOS (galactooligosaccharides), FOS (fructooligosaccharides), inulin, or resistant starch [11].
Step 3: Pair Prebiotics with Therapy
Prebiotics can amplify the benefits of psychological treatments. From June 2022 to March 2023, Dr. Robin M. Voigt at Rush University Medical Center led a 12-week study involving 70 veterans undergoing Cognitive Processing Therapy (CPT). Participants consumed prebiotic fiber bars - starting with one bar (10g fiber) daily in the first week and increasing to two bars (20g total) thereafter. The results showed that prebiotics improved the therapy’s effects on the gut microbiome by boosting SCFA-producing bacteria and reducing harmful, pro-inflammatory bacteria by the end of the trial [15][5]. This highlights how nutrition can enhance therapeutic outcomes.
For the best results, begin incorporating prebiotics during the first week of trauma-focused therapy. This aligns with the typical 12-week duration of PTSD treatment, giving your gut microbiota enough time to adapt and improve [15][5]. To support these efforts, stay hydrated, eat regular meals, and steer clear of alcohol [16][17].
"Targeting the intestinal microbiome through prebiotic supplementation could represent a promising avenue for enhancing treatment outcomes in some individuals with PTSD."
- Robin M. Voigt, PhD, Rush University Medical Center [14]
Using Begin Rebirth RE-1™ for PTSD Recovery
What Is Begin Rebirth RE-1™
Begin Rebirth RE-1™ is a specialized synbiotic designed to support PTSD recovery by targeting the gut microbiome. This 3-in-1 formula combines prebiotics, probiotics, and postbiotics to restore gut balance. Each sachet contains an impressive 500 billion CFU delivered through Human Origin Strains (HOSt™), ensuring effective colonization in the gut. The prebiotic mix includes inulin, resistant starch type 2, resistant maltodextrin, and rice bran, which fuel the production of short-chain fatty acids (SCFAs). To ensure these components reach the colon intact, the formula uses the Lyosublime™ delivery system, which protects the ingredients as they pass through the digestive tract [5].
How Begin Rebirth RE-1™ Helps PTSD Recovery
SCFAs are essential for reducing inflammation and maintaining the gut-brain connection, both of which are critical in PTSD recovery. Patients with PTSD often have lower levels of beneficial SCFAs and higher amounts of pro-inflammatory Gram-negative bacteria. Begin Rebirth RE-1™ works to boost SCFA production, helping to reduce brain inflammation and reestablish proper communication between the gut and the brain through pathways like the vagus nerve, HPA axis, and immune system [5]. Clinical studies have shown that this prebiotic formula can significantly alter microbiota composition in as little as 10 days [5].
"Targeting the intestinal microbiome through prebiotic supplementation could represent a promising avenue for enhancing treatment outcomes in some individuals with PTSD."
- Robin M. Voigt, PhD, Rush University Medical Center [5]
Recommended Reset Plans for PTSD Recovery
Begin Rebirth RE-1™ offers three reset plans tailored to different recovery needs and therapy timelines:
| Reset Plan | Duration | Best For |
|---|---|---|
| Rapid Reset | 7 Days | Quick microbiome adjustment to kickstart recovery |
| Standard Reset | 4 Weeks | Stabilizing SCFA production and strengthening the gut barrier |
| Comprehensive Reset | 12 Weeks | Long-term support alongside trauma-focused therapy |
The 12-week plan aligns with evidence-based PTSD therapies like Cognitive Processing Therapy (CPT), which typically involves 12 to 16 weekly sessions [5]. This period allows for meaningful microbiota shifts to complement the psychological benefits of therapy. For example, a 12-week clinical study led by Dr. Robin M. Voigt at Rush University Medical Center showed that this approach enhanced therapy outcomes in 70 veterans with PTSD. The study observed increased SCFA-producing bacteria and reduced inflammation markers, highlighting the benefits of combining microbiome resets with clinical interventions [5]. To maximize results, it’s recommended to start the reset during the first week of trauma-focused therapy, synchronizing gut health improvements with psychological treatment [5].
Conclusion
Focusing on gut health is a crucial step in supporting mental recovery for those dealing with PTSD. The connection between the gut and brain, known as the gut-brain axis, plays a major role in mental health. Research shows that the gut microbiome can explain about 48% of the variation in PTSD symptom severity [4]. By restoring gut balance with prebiotics, you can boost short-chain fatty acids (SCFAs), which help reduce neuroinflammation and regulate stress responses.
Targeted synbiotic solutions offer a practical way to speed up recovery. For example, Rebirth RE-1™ is a clinically supported synbiotic blend that can restore gut balance and increase SCFAs in just 10 days [5]. This makes it a powerful complement to therapies like Cognitive Processing Therapy (CPT), which are proven to aid in trauma recovery.
For the best results, pair prebiotic supplementation with evidence-based mental health treatments. If you're starting trauma-focused therapy, the 12-week Comprehensive Reset aligns well with typical therapy timelines, giving your gut microbiota enough time to make meaningful changes. Alternatively, the 7-day Rapid Reset is a great way to kick-start gut health improvements as part of your recovery journey.
Taking steps to improve gut health is a foundational part of mental wellness. Start by reviewing your diet, adding prebiotic-rich foods, and following a structured plan to reset your gut. With strong research backing the link between gut health and PTSD recovery, you now have the tools to take action. Combine these dietary strategies with therapy to unlock the full potential of gut-focused recovery.
FAQs
How can prebiotics support PTSD recovery through gut health?
Prebiotics, which are non-digestible fibers, play an important role in supporting the good bacteria in your gut. These beneficial bacteria produce short-chain fatty acids (SCFAs) and other compounds that communicate with the brain through the gut-brain axis. This connection helps reduce inflammation throughout the body, strengthens the gut lining, and regulates the hypothalamic-pituitary-adrenal (HPA) stress response - factors often disrupted in individuals with PTSD.
Studies suggest that prebiotics can enhance microbial diversity and restore gut balance, which may help alleviate PTSD-related symptoms like intrusive thoughts, heightened arousal, and mood swings. By encouraging SCFA production and improving gut-brain communication, prebiotics contribute to a healthier gut environment and better mental health.
If you're looking for an easy way to add prebiotics to your daily routine, Begin Rebirth RE-1™ offers a clinically supported 3-in-1 eubiotic synbiotic. This formula combines prebiotics, probiotics, and postbiotics to quickly reset your microbiome, reduce inflammation, and support pathways associated with PTSD symptoms - all in a simple, user-friendly protocol.
What are the best prebiotic foods to support PTSD recovery?
Incorporating foods rich in prebiotics into your meals can significantly support PTSD recovery by strengthening the gut-brain connection. Some excellent choices to include are:
- Vegetables: Onions, garlic, leeks, asparagus, and Jerusalem artichokes, which are packed with inulin.
- Whole grains: Options like oats, barley, and wheat provide resistant starch and beta-glucans.
- Fruits: Bananas, apples, and berries are great sources of fructooligosaccharides.
- Legumes: Lentils, chickpeas, and black beans offer a solid prebiotic boost.
Simply adding 1/2 to 1 cup of these foods to your daily diet can make a difference. For instance, you could start your morning with oatmeal topped with bananas and berries or enjoy roasted asparagus as a dinner side. These small changes can help feed the beneficial bacteria in your gut.
If meeting your prebiotic needs through food feels overwhelming, a supplement like Begin Rebirth RE-1™ could be a practical solution. This 3-in-1 eubiotic combines prebiotics, probiotics, and postbiotics to reset your microbiome, promoting balance and supporting mental health during PTSD recovery.
How do short-chain fatty acids (SCFAs) support PTSD recovery through the gut-brain connection?
Short-chain fatty acids (SCFAs) - such as acetate, propionate, and butyrate - are produced when prebiotic fibers are fermented by gut bacteria. These compounds play a key role in connecting gut health to brain function, particularly for individuals recovering from PTSD. SCFAs help fortify the intestinal barrier, reduce systemic inflammation, and regulate immune responses. This reduces the risk of neuroinflammation and supports mental wellness.
SCFAs also impact brain health by boosting neuroplasticity and aiding the production of critical neurotransmitters like serotonin and GABA, which are vital for maintaining mood balance. These combined effects can help regulate the body’s stress response, ease anxiety, and improve the processing of fear-based memories - factors that are crucial for PTSD recovery.
Adding prebiotics to your diet is an effective way to increase SCFA production and strengthen the gut-brain connection. Begin Rebirth RE-1™ is a research-supported 3-in-1 synbiotic that blends prebiotics, probiotics, and postbiotics to elevate SCFA levels, nurture gut health, and enhance emotional resilience. When used regularly, along with therapy, a nutritious diet, and stress-management techniques, it can aid in reducing PTSD symptoms and promoting overall mental well-being.