Struggling with sleep? Your gut might hold the answer. Research shows that psychobiotics - specific strains of bacteria targeting the gut-brain axis - can help improve sleep quality, regulate stress, and even support your body's natural rhythms. Here's how:
- Gut-Sleep Connection: The gut microbiome influences hormones like serotonin and melatonin, which are critical for sleep.
- Psychobiotic Strains: Bacteria like Lactobacillus helveticus and Bifidobacterium longum reduce stress and improve sleep quality.
- Two-Way Impact: Poor sleep disrupts gut health, while a balanced gut can promote restful sleep.
- Key Pathways: The vagus nerve, HPA axis, and immune system link gut microbes to brain functions that regulate sleep.
Emerging studies suggest psychobiotics and targeted supplements (like eubiotic synbiotics) could be game-changers for managing stress-related sleep issues. Pair these with a fiber-rich diet, regular exercise, and stress management to maximize results. While promising, more research is needed to refine the best strains and dosages for long-term benefits.
Clinical innovations in sleep, stress, and the gut-brain axis with Microbiome Labs & Fullscript
How the Gut-Brain Axis Regulates Sleep
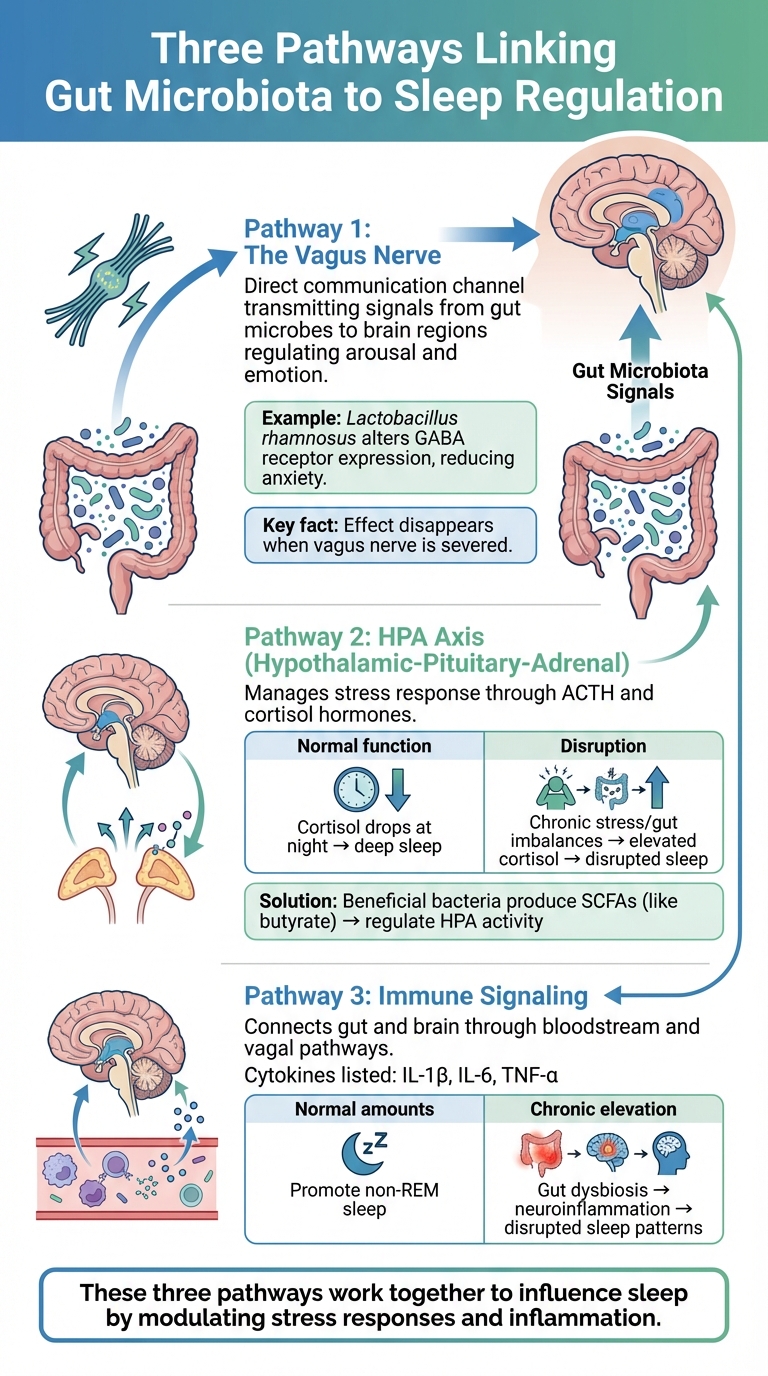
How the Gut-Brain Axis Regulates Sleep: Three Key Pathways
The gut-brain axis is a two-way communication system connecting the gut microbiota with the central nervous system. This intricate network relies on neural, hormonal, immune, and metabolic pathways to influence sleep-wake cycles [7][8]. When the gut microbiome is in balance, it sends signals that promote restful sleep. However, disruptions in this balance can lead to insomnia, fragmented sleep, and poor sleep quality. These interactions highlight how microbial signals can impact both circadian rhythms and neuroinflammation.
Primary Communication Pathways
Three key pathways link the gut microbiota to the brain's sleep regulation centers:
- The vagus nerve serves as a direct communication channel, transmitting signals from gut microbes to brain regions that regulate arousal and emotion. For example, Lactobacillus rhamnosus has been shown to alter GABA receptor expression in the brain, reducing anxiety-like behaviors. Notably, when researchers severed the vagus nerve in mice, this calming effect disappeared, demonstrating the nerve's essential role [7].
- The hypothalamic-pituitary-adrenal (HPA) axis manages the body’s stress response through hormones like ACTH and cortisol. Normally, cortisol levels drop at night to allow for deep sleep. However, chronic stress - often triggered by gut imbalances or inflammation - keeps cortisol levels elevated, leading to disrupted sleep. Beneficial gut bacteria produce short-chain fatty acids (SCFAs) like butyrate, which can help regulate HPA activity and alleviate stress-induced sleep issues [7].
- Immune signaling connects the gut and brain through the bloodstream and vagal pathways. Pro-inflammatory cytokines such as IL-1β, IL-6, and TNF-α, which are influenced by gut microbiota composition, can promote non-REM (NREM) sleep in normal amounts. But when these cytokines are chronically elevated due to gut dysbiosis, they contribute to neuroinflammation and disrupt healthy sleep patterns [7][8][9].
Together, these pathways provide insight into how gut microbes influence sleep by modulating both stress responses and inflammation.
Microbial Influence on Circadian Rhythms
Gut microbes don’t just impact sleep quality - they help regulate the body’s internal clock. Many gut bacteria exhibit diurnal rhythms, meaning their activity and metabolite production fluctuate throughout the day. These metabolites, particularly SCFAs like butyrate, play a role in regulating core clock genes (Per2, Bmal1) in tissues throughout the body, helping to stabilize circadian rhythms [7][8].
Animal studies have demonstrated this connection. When butyrate was administered to rodents, their NREM sleep increased by nearly 50%, linking microbial metabolites to deeper, more restorative sleep [7]. In humans, certain microbiota profiles - such as higher levels of Firmicutes, lower levels of Prevotella, and greater microbial diversity - are associated with better sleep quality. Prebiotics that encourage the growth of beneficial strains like Parabacteroides distasonis have also been shown to improve both sleep and circadian alignment [8].
Neuroinflammation and Sleep Quality
An imbalanced gut can lead to increased intestinal permeability, often referred to as "leaky gut." This allows bacterial components like lipopolysaccharides (LPS) to enter the bloodstream, triggering systemic inflammation. Elevated levels of pro-inflammatory cytokines can cross the blood-brain barrier, causing neuroinflammation that disrupts the balance of sleep-regulating neurotransmitters and cytokines [7][8][9]. This often results in fragmented sleep, reduced slow-wave sleep, and the heightened arousal seen in insomnia.
Experiments in mice have revealed that stool transplants from sleep-deprived, inflamed animals can transfer elevated inflammatory markers and altered sleep patterns to germ-free mice. Interestingly, this effect disappears when the vagus nerve is severed, emphasizing the combined roles of immune and vagal signaling in sleep disruption [7]. On the flip side, SCFAs, probiotics, and diets that support beneficial gut bacteria have been shown to reduce neuroinflammation and improve sleep efficiency. For instance, a clinical trial found that prebiotic yeast mannan increased the duration of NREM stage 3 sleep and total sleep time, which was linked to higher levels of fecal propionate and GABA [7][9].
Neurotransmitters and Metabolites Affected by Psychobiotics
Building on the gut-brain pathways we explored earlier, specific neurotransmitters and metabolites offer a clearer understanding of how psychobiotics influence sleep patterns. The key players here are serotonin, melatonin, GABA, and short-chain fatty acids (SCFAs), each contributing to sleep onset, quality, and continuity.
Serotonin, Melatonin, and Sleep Onset
Certain gut bacteria, particularly Lactobacillus and Bifidobacterium, play a role in increasing tryptophan availability, which boosts intestinal serotonin production. This serotonin acts as a precursor for melatonin synthesis in the pineal gland, helping regulate the circadian rhythm and supporting timely sleep onset [2]. Disruptions in melatonin timing - common in individuals with evening chronotypes - can throw off sleep-wake cycles. Psychobiotics that restore gut microbial balance may help normalize melatonin secretion by influencing circadian gene expression and reducing inflammation that impacts the brain’s internal clock [2][5]. Interestingly, animal studies show that external melatonin can reverse microbiota disruptions caused by sleep loss, highlighting a two-way relationship between melatonin and gut health [2].
GABA and Sleep Depth
Certain Lactobacillus and Bifidobacterium strains are known to produce GABA or enhance GABAergic signaling, which is linked to deeper non-REM sleep [2][3]. Human trials have shown that higher GABA levels, combined with reduced orexin and increased adenosine signaling, improve non-REM sleep quality and reduce insomnia symptoms. For example, a study from August 2021 found that Lactobacillus plantarum PS128™ supplementation over eight weeks helped high-stress air force personnel by reducing insomnia severity and salivary cortisol, while also improving mental health. Researchers attributed these effects to increased GABA levels and better regulation of the HPA axis [3]. Similarly, Bifidobacterium longum 1714 demonstrated improvements in sleep quality scores (p=0.01) and reduced daytime dysfunction (p<0.05) after four weeks in healthy adults. It also extended sleep duration (≥6 hours) in stressed students during exams [4]. Beyond GABA, metabolites like SCFAs also play a role in connecting gut activity to sleep regulation.
Short-Chain Fatty Acids (SCFAs) and Sleep
SCFAs - acetate, propionate, and butyrate - are produced when gut microbes ferment dietary fibers [2]. These molecules influence circadian rhythms, histone acetylation, and metabolic and immune pathways that are tied to sleep cycles [2]. By regulating inflammatory responses and energy balance, SCFAs help stabilize sleep patterns and improve sleep efficiency. Research shows that interventions that boost SCFA production - such as prebiotics, probiotic lactic acid bacteria (LAB) strains, and postbiotic butyrate - can correct gut imbalances and enhance sleep outcomes [2][10]. In rodent studies, specific prebiotic mixes have been shown to increase non-REM sleep, improve REM rebound, and reduce stress-induced body temperature changes, all pointing to better sleep regulation through SCFA pathways [10]. Products like the 3-in-1 eubiotic synbiotic Begin Rebirth RE-1™ have been shown to restore microbiome balance, boosting neurotransmitter and SCFA production to support better sleep [2][3][4]. Together, these chemical messengers illustrate the deep connection between gut health and sleep regulation.
sbb-itb-1bbfe7f
Research Evidence on Psychobiotics and Sleep
Recent research offers both clinical and preclinical insights into how psychobiotics may influence sleep patterns and quality.
Human Studies on Psychobiotics and Sleep
A randomized trial conducted in 2021 revealed that eight weeks of supplementation with Lactobacillus plantarum PS128™ reduced insomnia severity and decreased salivary cortisol levels in high-stress workers. These benefits were attributed to the modulation of the HPA axis and enhanced GABA signaling[3]. While the study did not include objective measurements of sleep stages, the drop in cortisol suggests a meaningful improvement in the stress-sleep dynamic.
In another double-blind trial from 2024, participants with sleep complaints received Bifidobacterium longum 1714 for eight weeks. The results showed improved Pittsburgh Sleep Quality Index (PSQI) scores, reduced daytime dysfunction, and better energy and social engagement (p ≤ 0.05). However, actigraphy data did not reveal significant changes in sleep patterns[4]. A 2023 meta-analysis further highlighted that daily intake of Lactobacillus gasseri BR-LAC-343 enhanced sleep quality among adults with mild to moderate stress. Additionally, research on Lactobacillus helveticus and Bifidobacterium longum strains demonstrated reduced anxiety and cortisol levels after one month, indirectly supporting sleep by alleviating stress responses[1].
Findings from Animal Studies
Animal models have been instrumental in uncovering the biological pathways connecting gut microbes to sleep regulation. Studies show that Lactobacillus and Bifidobacterium strains can elevate gut-derived GABA, serotonin, and short-chain fatty acids (SCFAs), all of which play roles in promoting non-REM (NREM) sleep and maintaining sleep continuity[2]. Sleep-deprived animals often experience a decline in these beneficial bacteria, potentially worsening gut dysbiosis.
Research in rodents also indicates that psychobiotics can lower orexin levels while increasing adenosine in specific brain regions, promoting deeper, more restorative sleep[3]. These findings align with earlier evidence that microbial metabolites influence sleep regulation. Moreover, studies involving melatonin supplementation in sleep-deprived animals emphasize the two-way relationship between gut microbes and circadian rhythms[2]. However, limitations in these animal studies, such as variability in design, highlight the need for further investigation.
Research Gaps and Future Directions
Despite encouraging results, research on psychobiotics and sleep has notable limitations. Many human trials have involved small sample sizes and focused on specific groups, such as stressed workers or individuals with mild sleep disturbances, which restricts the generalizability of findings[3][4]. Additionally, the observed effects are often strain-specific and relatively modest. For instance, while B. longum 1714 showed subjective improvements, it did not produce significant changes in actigraphy data. Similarly, another strain, JB-1, failed to outperform placebo in improving sleep[3][4]. The reliance on subjective measures like the PSQI, without complementary tools such as polysomnography, makes it challenging to assess changes in sleep architecture.
To address these gaps, future research should focus on larger, multi-center randomized controlled trials with standardized protocols. Combining subjective assessments with objective tools like actigraphy and polysomnography will provide a clearer picture of how psychobiotics influence sleep. Additionally, integrating advanced techniques such as microbiome sequencing, metabolomics, and neuroimaging could uncover how microbial changes impact circadian rhythms, melatonin production, and clock gene expression[2][3][4]. These approaches will help establish stronger evidence for the role of psychobiotics in sleep regulation.
Applying Research to Sleep Improvement
Eubiotic Synbiotics for Gut–Brain Support
Recent research highlights the potential of eubiotic synbiotics, such as Begin Rebirth RE-1™, to improve sleep by restoring gut balance and boosting the production of SCFAs, GABA, and serotonin precursors. This is achieved through a 3-in-1 formula combining prebiotics, probiotics, and postbiotics, delivering 500 billion CFU per serving with Human Origin Strains (HOSt™). Key strains like Lactobacillus gasseri BR-LAC-343 have been shown to enhance sleep quality in adults dealing with mild to moderate stress [1]. Other strains, including Lactobacillus helveticus BR-MCC1848 and Bifidobacterium longum BR-BB536, play a role in emotional balance by supporting GABA production and reducing cortisol levels. Additionally, the formula contains 4.5 g of prebiotic fibers (GOS and inulin) to feed beneficial gut bacteria and boost short-chain fatty acid production [1].
For optimal results, take one sachet each morning. Studies suggest that improvements in sleep quality and daytime functioning may appear after about four weeks, with peak benefits seen after eight to 12 weeks of consistent use. The Lyosublime™ delivery system ensures effective absorption throughout the gut without the need for refrigeration [1]. Pairing synbiotic supplementation with a nutrient-rich diet can further enhance sleep regulation.
Diet and Lifestyle for Better Sleep
Boosting dietary fiber intake to 25–30 g daily with foods like beans, lentils, asparagus, Jerusalem artichokes, onions, and garlic can nourish beneficial gut bacteria and promote better sleep. Foods containing galactooligosaccharides (GOS) and inulin are particularly helpful in producing metabolites linked to improved sleep health.
Adopting a Mediterranean-style diet, rich in vegetables, fruits, whole grains, legumes, nuts, and olive oil, can enhance microbial diversity and support sleep. On the other hand, limiting ultra-processed foods, excessive added sugars, and heavy meals close to bedtime helps maintain a healthy circadian rhythm. Sticking to consistent meal times - with the majority of calories consumed earlier in the day - further supports the alignment of both your body’s and gut microbiome’s circadian rhythms [2]. This dietary approach complements the benefits of targeted synbiotic use.
Incorporating regular physical activity - such as 20–30 minutes of moderate exercise on most days - also contributes to better sleep and a healthier gut microbiome. Coupling this with a consistent sleep-wake schedule, even on weekends, helps regulate the central and peripheral clocks that interact with microbial rhythms. Stress management is another key element, as it reinforces gut-brain alignment and improves sleep quality.
Managing Stress and Restoring Microbiome Balance
Chronic stress can disrupt sleep by activating the HPA axis, which increases cortisol levels, compromises gut barrier integrity, reduces beneficial gut bacteria, and triggers inflammation [2]. Techniques like mindfulness meditation, diaphragmatic breathing, and cognitive-behavioral strategies have been proven effective in lowering stress and improving sleep.
Incorporating daily relaxation practices can help maintain a healthy gut barrier. During particularly stressful periods, combining these practices with a psychobiotic or eubiotic synbiotic regimen may provide additional support for gut health and sleep quality.
To track progress, consider keeping a weekly journal of your bedtime, wake time, night awakenings, and overall daytime energy levels. This can help you identify patterns similar to those seen in clinical sleep studies [4]. It's important to remember that psychobiotics work best as part of a comprehensive approach to sleep improvement. For individuals with severe sleep issues, significant psychiatric conditions, or those on multiple medications, consulting a healthcare professional before starting a high-dose synbiotic regimen is highly recommended.
Conclusion
The connection between your gut microbiome and sleep quality is undeniable. Studies reveal that specific strains like Lactobacillus and Bifidobacterium play a key role in improving sleep by influencing the gut-brain axis. These bacteria produce essential neurotransmitters and metabolites that support better sleep. For instance, human trials have shown that strains such as Bifidobacterium longum 1714 and Lactobacillus plantarum PS128 can enhance sleep quality, reduce insomnia, and improve daytime functioning, particularly in individuals dealing with chronic stress [3][4].
Still, psychobiotics are most effective when part of a broader strategy. Since poor sleep can aggravate gut imbalances, addressing this cycle requires a holistic approach. Pairing synbiotic supplements with a fiber-rich diet, consistent sleep routines, stress management techniques, and regular physical activity can help support both the microbiome and restorative sleep. This multi-faceted approach not only disrupts the cycle of dysbiosis but also sets the stage for further advancements in this field.
Research is continually refining these methods, exploring the best strains, dosages, and long-term effects. Psychobiotics are emerging as valuable tools, particularly for those struggling with stress-related sleep issues [6][10]. However, for individuals with severe sleep disorders or underlying psychiatric conditions, consulting with a healthcare professional is crucial to ensure psychobiotics complement existing treatments rather than replace them.
The relationship between gut health and sleep represents an exciting area of discovery. By leveraging the power of the gut-brain axis, psychobiotics open up new possibilities for improving circadian rhythms, mood, and overall well-being. As research progresses, the ability to personalize microbiome-based interventions will only deepen the connection between gut health and quality sleep.
FAQs
How do psychobiotics help improve sleep quality?
Psychobiotics can improve sleep quality by nurturing a healthy gut microbiome, which is deeply connected to the gut-brain axis. This connection influences circadian rhythms - the internal clock that manages your sleep-wake cycles.
Some strains, such as Human Origin Strains (HOSt™), are especially effective at stabilizing the microbiome and minimizing disturbances in these rhythms. Over time, this can promote more consistent and restorative sleep.
How does the gut-brain connection impact sleep and wake cycles?
The connection between the gut and brain plays a key role in managing sleep-wake cycles. This link ties gut microbiota to brain function, influencing circadian rhythms - our body's internal clock - and aiding in the production of neurotransmitters like serotonin, which directly affect sleep quality.
Beyond that, the gut-brain axis also supports immune health and helps reduce inflammation, both of which can influence how well we sleep. Keeping your gut microbiome balanced is crucial for achieving restful sleep and maintaining overall health.
Can improving your diet and lifestyle boost the impact of psychobiotics on sleep quality?
Yes, adjusting your diet and lifestyle can boost how well psychobiotics work to support better sleep. Eating a balanced diet filled with fiber, whole foods, and essential nutrients helps keep your gut microbiome in good shape. This connection is crucial because a healthy gut directly impacts the gut-brain axis and your body's natural sleep-wake rhythms.
Adding habits like staying active, managing stress effectively, and sticking to a consistent sleep schedule can further enhance the impact of psychobiotics. Together, these steps can promote healthier sleep patterns and contribute to your overall well-being.