Probiotics can help reduce gut inflammation by rebalancing gut bacteria, strengthening the intestinal lining, and regulating immune responses. When your gut microbiome is out of balance, harmful bacteria can take over, leading to inflammation that affects your entire body. Probiotics counter this by promoting the growth of good bacteria, improving the gut barrier to prevent toxins from leaking into the bloodstream, and calming an overactive immune system.
Key Takeaways:
- Gut Microbiome Balance: Probiotics compete with harmful bacteria, lower gut pH, and release antimicrobial compounds to restore balance.
- Stronger Gut Barrier: They increase tight junction proteins and stimulate mucus production to protect the intestinal lining.
- Immune Regulation: Probiotics reduce inflammatory markers like TNF-α while boosting anti-inflammatory signals such as IL-10.
Clinical studies show that specific probiotic strains, like Lactobacillus rhamnosus GG and Escherichia coli Nissle 1917, can improve conditions like Ulcerative Colitis and reduce inflammation markers like C-reactive protein (CRP). You can incorporate probiotics through fermented foods (e.g., yogurt, kefir, sauerkraut) or supplements for higher doses.
To maximize benefits, pair probiotics with prebiotic-rich foods, maintain a high-fiber diet (21–38 grams daily), and avoid processed foods high in sugar and saturated fats.
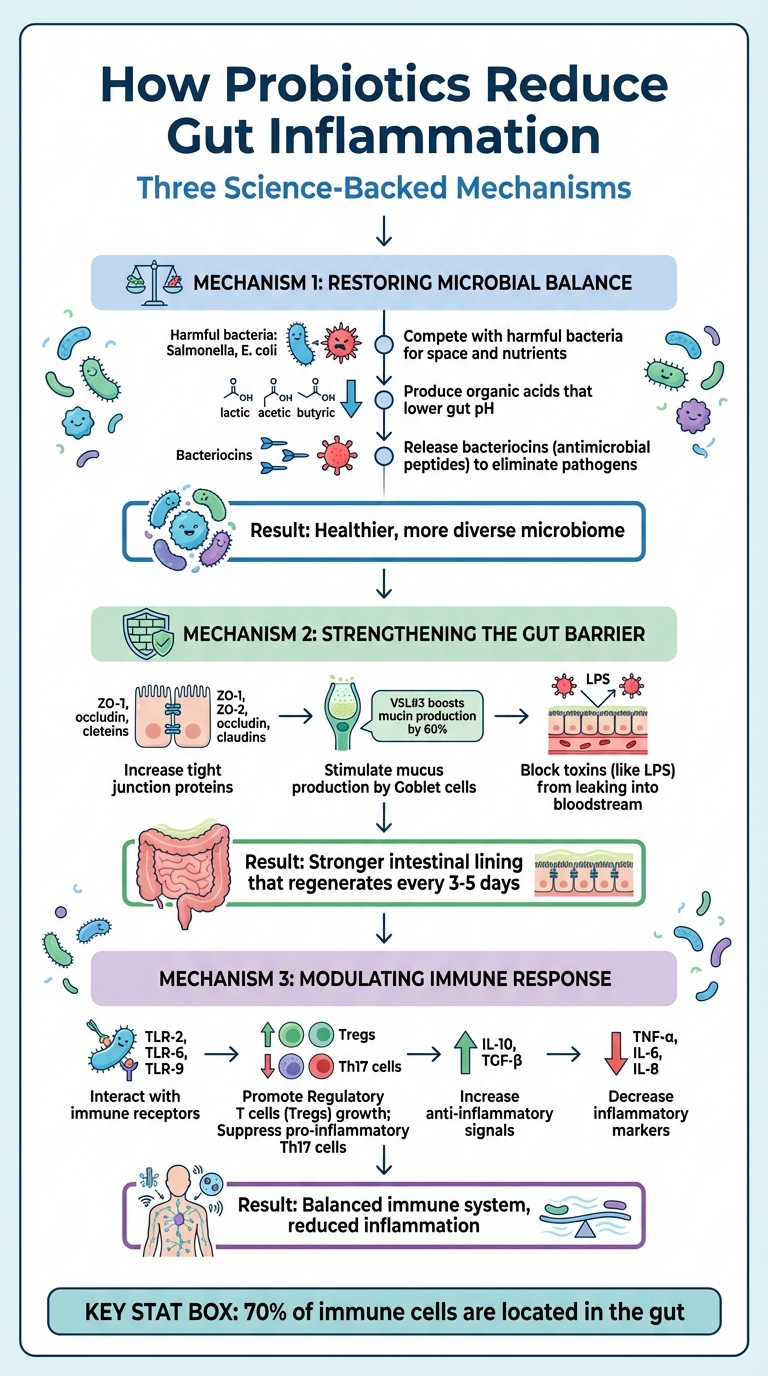
How Probiotics Reduce Gut Inflammation: 3 Key Mechanisms
Probiotic supplementation enhances intestinal immune cell response to curb inflammation
How Probiotics Reduce Gut Inflammation
Probiotics work in three primary ways to ease gut inflammation: balancing gut bacteria, strengthening the intestinal barrier, and adjusting immune system responses. These mechanisms address the underlying issues of inflammation, rather than just alleviating symptoms.
Restoring Microbial Balance
An imbalance in gut bacteria, known as dysbiosis, often leads to inflammation, especially when harmful bacteria like Salmonella or E. coli dominate. Probiotics help by competing with these pathogens for space and nutrients in the gut [2][4]. They also produce organic acids like lactic, acetic, and butyric acid, which lower the gut's pH, creating an environment where harmful bacteria struggle to survive [2][4].
Some probiotic strains take it further by releasing bacteriocins, which are antimicrobial peptides that actively eliminate harmful bacteria. This action helps beneficial microbes regain control, fostering a healthier and more diverse microbiome. Along with rebalancing bacteria, probiotics also play a role in strengthening the gut's physical defenses.
Strengthening the Gut Barrier
Your intestinal lining acts as a selective filter, allowing nutrients to pass through while blocking harmful substances. Probiotics bolster this barrier by increasing tight junction proteins like ZO-1, ZO-2, occludin, and claudins. These proteins "zip" intestinal cells together, preventing toxins such as lipopolysaccharides (LPS) from leaking into the bloodstream and causing inflammation [5][2].
Probiotics also stimulate Goblet cells to produce more mucus, which acts as a protective layer against harmful microbes. For instance, the probiotic formula VSL#3 was shown to boost mucin production by 60% in rat studies [5]. Strains like Escherichia coli Nissle 1917 and Lactobacillus plantarum 299v are particularly effective at enhancing mucin genes (MUC2, MUC3), which thicken this protective layer [5][2]. Since the intestinal lining regenerates every 3 to 5 days, probiotics support this natural renewal process, keeping the gut barrier strong and functional. Beyond physical protection, probiotics also fine-tune the immune system to further reduce inflammation.
Modulating the Immune Response
Probiotics interact with immune cell receptors, such as Toll-like receptors (TLR-2, TLR-6, and TLR-9), to initiate anti-inflammatory signaling pathways [3][6]. This helps shift the immune system from a hyperactive state to a more controlled and balanced one.
They also encourage the growth of Regulatory T cells (Tregs), which help prevent overactive immune responses. At the same time, probiotics suppress pro-inflammatory Th17 cells, which can harm the intestinal lining [3][2]. This results in a healthier cytokine balance: an increase in anti-inflammatory signals like IL-10 and TGF-β, and a reduction in inflammatory markers such as TNF-α, IL-6, and IL-8 [3][7].
One standout example is Lactobacillus reuteri ATCC PTA 6475, which contains the hdcA gene. This gene converts L-histidine into histamine, which then binds to H2 receptors on immune cells, suppressing TNF-α production - a major driver of inflammation [7]. Clinical studies on patients with non-alcoholic fatty liver disease (NAFLD) showed that probiotics increased CD8+ T cells, which helped regulate immune functions and reduced intestinal permeability [2].
Scientific Evidence for Probiotics and Gut Inflammation
There’s solid clinical evidence showing that probiotics can help reduce gut inflammation, backed by studies and trials that highlight their effectiveness.
Clinical Studies on Probiotic Strains
Research has shown that certain probiotic strains can significantly reduce markers of inflammation in the gut. For instance, an umbrella meta-analysis of randomized controlled trials found that probiotics lowered C-reactive protein (CRP) - a key inflammation marker - with an effect size of -1.02. The same analysis also reported reductions in pro-inflammatory cytokines such as TNF-α (effect size -0.35) and IL-6 (effect size -0.36) [9]. These results suggest that probiotics could play a targeted role in clinical interventions for inflammation-related conditions.
Specific trials have also demonstrated the effectiveness of probiotics in treating gut disorders. For example, a randomized double-blind study involving Escherichia coli Nissle 1917 alongside mesalazine in Ulcerative Colitis (UC) patients showed that the probiotic group had better outcomes, including lower partial Mayo scores and higher rates of endoscopic remission, compared to those receiving mesalazine alone [4]. Another trial by Pagnini et al. found that Lactobacillus rhamnosus GG improved both clinical activity and endoscopic scores in UC patients over a four-week period [4]. Similarly, a study by Bamola et al. highlighted the benefits of Bacillus clausii UBBC-07 in UC and Crohn's Disease patients, reporting increased levels of anti-inflammatory cytokines, reduced pro-inflammatory markers, and a boost in beneficial bacteria like Faecalibacterium [4].
Effects on Chronic Gut Conditions
Probiotics have shown promise in managing chronic gut conditions, particularly Ulcerative Colitis and pouchitis. Restoring microbial balance and improving gut barrier function appear to be key mechanisms behind these benefits. Multi-strain formulations like VSL#3 and single strains such as Bifidobacterium longum 536 have been effective in inducing and maintaining remission in UC [8]. For instance, in children with UC, VSL#3 reduced the relative risk of relapse to 0.32 within a year [8]. Another study found that Lactobacillus rhamnosus GG was as effective as mesalazine in delaying UC relapses [8].
"The use of probiotics and/or synbiotics has positive effects in the treatment and maintenance of UC, whereas in CD clear effectiveness has only been shown for synbiotics."
- Maria Jose Saez-Lara et al., University of Granada [8]
For Crohn's Disease, the evidence supporting probiotic monotherapy is less robust. However, synbiotics - combinations of probiotics and prebiotics - have demonstrated more consistent results. This aligns with probiotics’ ability to modulate the immune system and enhance gut barrier integrity. In one trial by Valcheva et al., 25 UC patients were treated with oligofructose-enriched inulin for nine weeks. The high-dose group (15 g per day) achieved a 77% clinical response and remission rate, compared to 33% in the low-dose group [4]. Additionally, studies combining Bifidobacterium longum with the prebiotic Synergy 1 showed improved symptoms and reduced inflammation in Crohn's Disease patients [8].
sbb-itb-1bbfe7f
Adding Probiotics to Your Daily Routine
Including probiotics in your daily routine can help reduce gut inflammation and improve overall digestive health. You can achieve this through fermented foods or specialized supplements.
Food Sources of Probiotics
Fermented foods are a simple and natural way to introduce helpful bacteria into your gut. For instance, yogurt with live and active cultures is widely available and often contains Lactobacillus strains, which support digestion. Kefir, a fermented milk drink, offers an even broader range of bacterial strains, promoting greater microbial diversity.
Other excellent options include sauerkraut and kimchi, both rich in lactobacilli. When shopping for these, make sure to choose unpasteurized versions labeled with "live and active cultures", as pasteurization destroys the beneficial bacteria. Similarly, when buying pickles, look for those fermented in saltwater rather than vinegar, as vinegar-based pickles lack live probiotics.
While these foods are packed with vitamins, minerals, and natural prebiotics, they generally provide lower concentrations of specific probiotic strains compared to supplements. However, they can work alongside supplements to enhance your gut health.
Probiotic Supplements for Targeted Support
Supplements are a practical option when you need higher doses of probiotics for specific concerns like gut inflammation. They deliver concentrated strains and quantities that food alone may not provide.
Begin Rebirth RE-1™ (https://beginrebirth.com) is an example of a supplement designed for intensive microbiome support. Each serving contains 500 billion CFU and Human Origin Strains (HOSt™), along with 4.5 grams of prebiotic fiber (GOS and inulin). This combination creates a synbiotic effect, enhancing the survival and activity of beneficial bacteria. This targeted approach is especially helpful after antibiotic treatments or during high-stress periods, when your gut microbiome may need extra support.
Tips for Maximizing Probiotic Effectiveness
To get the most out of probiotics, timing and pairing are key. Many experts recommend taking probiotics on an empty stomach, as lower stomach acid levels may improve their survival. However, some strains may work better when taken with food. If you're on antibiotics, take your probiotic dose at least two hours apart to ensure the beneficial bacteria remain effective.
Pairing probiotics with prebiotics can further boost their benefits. Foods like onions, garlic, bananas, and chicory root contain prebiotic fibers that feed the good bacteria in your gut. Considering that most Americans consume only about 16.2 grams of fiber daily - far below the recommended 21–38 grams - incorporating more fiber-rich foods is a smart move. A good rule of thumb is to choose packaged foods with a total carbohydrate-to-fiber ratio of less than 10:1 [10].
"Nutrition is the main therapeutic tool to positively influence the microbiome. A diet rich in fiber, vegetables, and fruit helps establish a varied and rich microbiome that promotes the health of the host."
- David Rakel, MD, University of Wisconsin-Madison [10]
Consistency is crucial. Probiotics need to be consumed regularly to maintain their presence in your gut and deliver long-term benefits [10]. Keep in mind, you might experience temporary side effects like digestive discomfort, headaches, or constipation as your gut adjusts [2]. To maximize benefits, avoid excessive processed foods high in saturated fats and sugars, and focus on managing stress levels, both of which can negatively impact gut health [3].
Conclusion
Gut inflammation doesn’t have to be a lifelong struggle. Probiotics offer a well-researched way to help restore balance in your digestive system. These beneficial bacteria tackle gut inflammation by addressing the root causes. They crowd out harmful microbes, strengthen the intestinal lining by boosting tight junction proteins like ZO-1 and occludin, and guide immune cells toward anti-inflammatory activity.
Consider this: about 70% of your immune cells are located in your gut [3]. That means a healthy microbiome impacts more than just digestion - it plays a key role in your overall well-being. The connection between gut health and whole-body wellness is undeniable.
Consistency is crucial for results. Whether you opt for fermented foods, a high-quality supplement like Begin Rebirth RE-1™ (featuring 500 billion CFU and Human Origin Strains), or a mix of both, sticking to a daily routine is what makes the difference. Clinical studies show that noticeable improvements can happen within weeks [4][1], so patience and regularity are just as important as the probiotics themselves.
To maximize your efforts, combine probiotics with prebiotic-rich foods, ensure you’re getting enough fiber (21–38 grams per day), and cut back on processed foods, saturated fats, and added sugars. While your gut microbiome is naturally resilient, it thrives best when given the right conditions.
Start your daily probiotic routine today and take an active step toward better gut and overall health.
FAQs
How do probiotics help strengthen the gut barrier?
Probiotics play a crucial role in strengthening the gut barrier by enhancing the tight junctions - the connections between intestinal cells. They encourage the production of essential proteins and mucins, which help fortify the gut lining and reduce its permeability. This makes it harder for harmful substances like bacteria and toxins to pass into the bloodstream, where they can spark inflammation.
Specific probiotic strains, such as Lactobacillus and Bifidobacterium, also aid in renewing intestinal cells, which contributes to a stronger and healthier gut barrier. By supporting these functions, probiotics help maintain gut harmony, lower inflammation, and improve immune system performance.
What’s the best way to add probiotics to my diet?
Incorporating probiotics into your daily routine doesn’t have to be complicated. Start with probiotic-rich foods like yogurt, kefir, sauerkraut, and kimchi - these fermented options are packed with beneficial bacteria that help maintain gut health.
If you’re looking for an extra boost, high-quality probiotic supplements are a great option. These are typically available in capsules or sachets. When choosing a supplement, focus on products with clinically supported strains and the right CFU (colony-forming units) count. For instance, Begin Rebirth RE-1™ combines prebiotics, probiotics, and postbiotics to help reset and optimize your microbiome.
To get the most out of probiotics, pair them with prebiotics, which are fibers that nourish good bacteria. Foods like garlic, onions, bananas, and whole grains are excellent choices. Combining these with a well-rounded diet can help nurture your gut microbiome and manage inflammation effectively.
Can probiotics help with other health conditions besides gut inflammation?
Probiotics do more than just address gut inflammation - they can play a part in supporting various health conditions. By promoting a balanced gut microbiome, they may positively impact immune function and overall health. Studies suggest probiotics could help manage conditions tied to immune system activity and systemic inflammation, including inflammatory bowel disease (IBD), cardiovascular concerns, and even obesity.
Additionally, probiotics may influence the gut-brain connection, offering potential benefits for mental and neurological health. Their role in regulating immune responses goes beyond the digestive system, emphasizing their potential to support immune health and reduce inflammation throughout the body.