Your gut health directly impacts your immune system - 70% to 80% of immune cells reside in your gut. When this balance is disrupted, it can lead to chronic inflammation, digestive issues, and even systemic problems like fatigue, allergies, and mental health challenges. Postbiotics, the non-living byproducts of beneficial bacteria, offer a targeted solution by strengthening the gut barrier, reducing inflammation, and supporting immune function.
Key Takeaways:
- What are Postbiotics? They are bioactive compounds (like short-chain fatty acids) produced by beneficial bacteria during fermentation. Unlike probiotics, postbiotics are non-living and more stable.
- How They Help: Postbiotics improve gut lining integrity, modulate inflammation, and enhance immune responses without the risks associated with live probiotics.
- Symptoms of Gut-Immune Imbalance: Bloating, fatigue, frequent infections, weight changes, and mood swings are common signs.
- Causes of Imbalance: Poor diet, antibiotic overuse, stress, and lifestyle factors can disrupt gut health.
- Clinical Evidence: Studies show postbiotics can reduce inflammation, improve gut health, and even enhance drug absorption.
Postbiotics are a safe, effective option to restore gut-immune balance, especially for vulnerable groups. Products like Begin Rebirth RE-1™ combine prebiotics, probiotics, and postbiotics for a complete gut health solution.
184: Postbiotics & Immune Health – Dr. Justin Green & Keri Gans
What Is Gut-Immune Imbalance?
Gut-immune imbalance, also known as dysbiosis, happens when the delicate balance between gut microbes and immune cells is disrupted [1][10]. This disruption interferes with the communication between gut bacteria and immune cells, causing the body to lose its ability to maintain "immunological homeostasis" - essentially, the capacity to differentiate between actual threats and harmless substances [10].
The effects of this imbalance go far beyond the digestive system. A well-balanced gut helps maintain a healthy "inflammatory tone", meaning the immune system stays alert but doesn't overreact. When dysbiosis occurs, this balance is thrown off, weakening the gut barrier and triggering a chain reaction of systemic problems. Beneficial microbes diminish, harmful bacteria take over, and the result is chronic low-grade inflammation, increased intestinal permeability (commonly referred to as "leaky gut"), and an immune system that either overreacts or underreacts when it shouldn't [1][2].
"Immune homeostasis is achieved and maintained due in part to the extensive interplay between the gut microbiota and host mucosal immune system."
- C T Peterson, The George Washington University [10]
Here’s some perspective: the human gut contains an estimated 10^13 bacteria, making it the densest microbial ecosystem known to science [10]. These microbes collectively encode about 150 times more genes than the human genome [10]. When this intricate system becomes unbalanced, the consequences can be severe. In fact, noncommunicable diseases tied to gut-immune dysregulation and chronic inflammation were responsible for 74% of global deaths in 2020 [2]. That year alone, cardiovascular disease claimed 17.9 million lives, while cancer caused 9.3 million deaths [2].
What Causes Gut-Immune Imbalances?
Several factors can disturb the gut ecosystem, with diet being one of the most influential. Diets high in fat and refined carbohydrates reduce beneficial bacteria and encourage harmful strains [5][10]. Similarly, a lack of dietary fiber leaves gut microbes "starving", which can weaken the intestinal barrier and spark inflammation.
Antibiotics are another major disruptor. While they can be life-saving, broad-spectrum antibiotics can wipe out 25% to 50% of bacterial species in just 24 hours [10][11]. This creates a vacuum where harmful, inflammation-promoting bacteria can thrive. Children are particularly vulnerable - antibiotic use before age three has been linked to reduced microbial diversity and an increased risk of asthma, obesity, and inflammatory bowel disease later in life [12].
Modern lifestyle factors also play a role. Chronic stress, sedentary habits, and urban living all contribute to a less diverse microbiome [1][2]. Even the way a baby is born can have lasting effects: C-section deliveries often result in colonization by skin-associated bacteria like Staphylococcus instead of the beneficial microbes typically passed on during vaginal delivery. This can lead to reduced microbial diversity and a less robust immune system early in life [10]. Over time, these disruptions can erode the gut's natural resilience, making recovery from challenges harder and potentially locking the system into a state of dysbiosis [10][11].
"The human gut microbiota displays high interpersonal variation but is stable over time, displaying resilience in the face of perturbing influences such as dietary flux and exposure to antibiotics."
- S. N. Peterson, Professor, Sanford-Burnham Medical Research Institute [10]
Common Symptoms of Gut-Immune Imbalance
The symptoms of gut-immune imbalance aren't confined to digestive issues. While digestive problems like bloating, constipation, diarrhea, and abdominal discomfort are common [1][6], the effects can extend throughout the body. Chronic low-grade inflammation may leave you feeling persistently fatigued, and the immune system might become overly sensitive or sluggish, leading to frequent infections, allergies, or even autoimmune reactions [1][12].
Metabolic issues can also emerge. Dysbiosis can contribute to unexplained weight gain, insulin resistance, and nutrient absorption problems. The large intestine, home to 10^11 to 10^12 bacteria per gram, may become less effective at extracting nutrients and producing important compounds [4]. Globally, over 800 million adults live with diabetes, and obesity rates in the U.S. have reached 40.3% as of 2023 - both conditions closely linked to gut-immune imbalance [13].
Perhaps most striking is the impact on mental health. Since about 90% of serotonin is produced in the gut, disruptions in the microbiome can destabilize mood [1]. The gut-brain axis connects dysbiosis to anxiety, depression, and even behavioral changes [12][3]. These effects aren't just coincidental - they reflect changes in neurotransmitter production and inflammatory signals between the gut and brain.
| Symptom Category | Common Manifestations |
|---|---|
| Digestive Issues | Bloating, constipation, abdominal discomfort, IBS symptoms [1][4] |
| Immune Dysfunction | Frequent infections, allergies, autoimmune conditions [1][10] |
| Systemic/Metabolic | Chronic fatigue, inflammation, obesity, insulin resistance [1][2] |
| Mental/Neurological | Mood swings, anxiety, depression (linked to serotonin changes) [1][5] |
The long-term risks of gut-immune imbalance are serious. Persistent dysbiosis can pave the way for chronic illnesses like Type 2 diabetes, inflammatory bowel disease, cardiovascular disease, and non-alcoholic fatty liver disease [2][13]. However, there’s hope - lifestyle choices like diet and stress management play a much larger role in shaping gut health than genetics, which accounts for only 10% to 20% of microbial diversity [13].
Next, we’ll explore how postbiotics can help address these imbalances.
What Are Postbiotics?
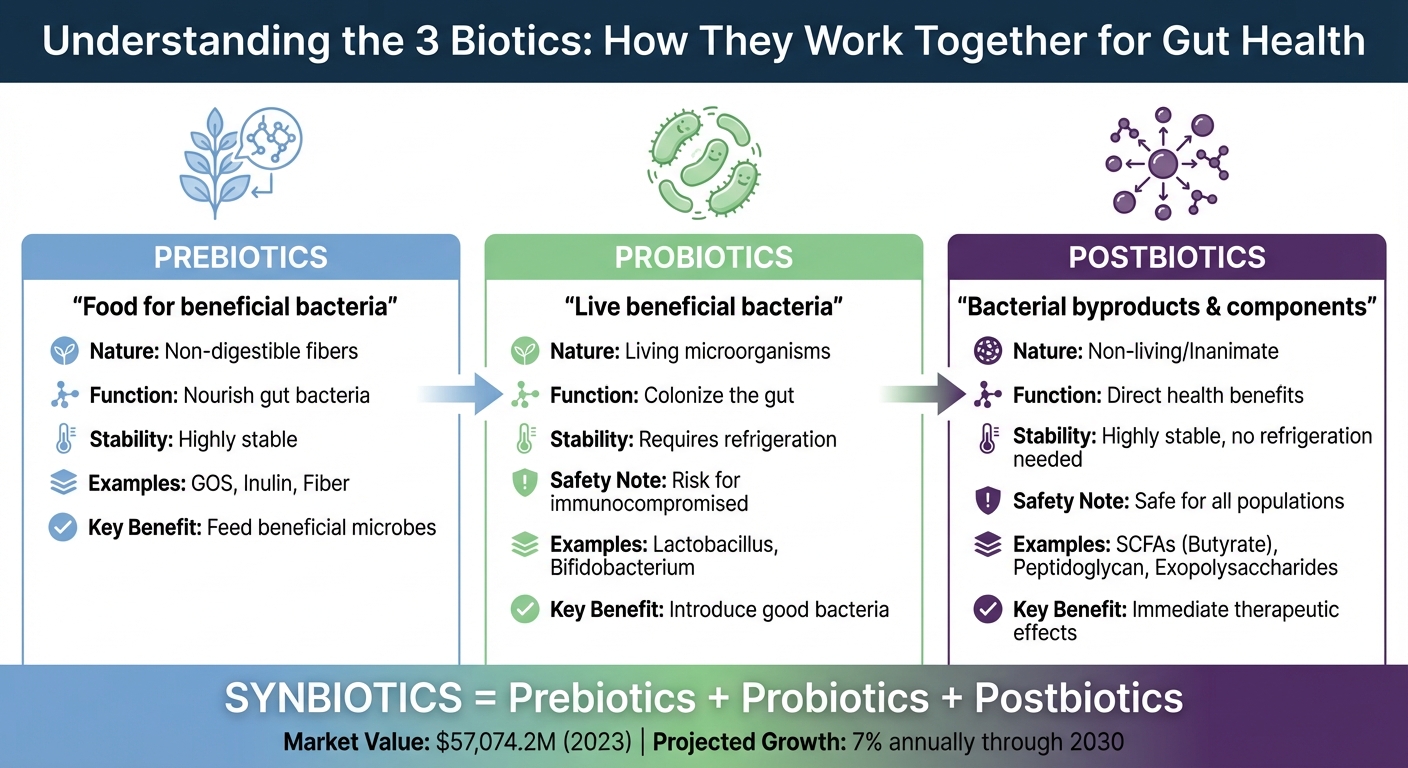
Prebiotics vs Probiotics vs Postbiotics: Key Differences and Benefits
Postbiotics are essentially the non-living byproducts of microorganisms, created during fermentation, that can positively impact health. Defined as "preparations of inanimate microorganisms and/or their components that confer a health benefit on the host" [2], they include the beneficial compounds bacteria produce while breaking down food, as well as parts of the bacterial cells themselves. Unlike probiotics, which are live bacteria, postbiotics are non-living, making them more stable under various conditions. This stability means they don’t require refrigeration, making them easier to handle and safer for groups like infants, the elderly, or those with weakened immune systems. They also avoid risks like bacterial translocation or the spread of antibiotic resistance genes [2].
"Postbiotics are superior to probiotics because of their purity, ease of preparation, long shelf life, mass production capability, and more targeted responses."
- Nataraj et al. [3]
Here’s the key difference: probiotics introduce live bacteria to your gut, prebiotics act as the food for those bacteria, and postbiotics deliver the beneficial byproducts and cellular components that directly support your health. According to the International Scientific Association of Probiotics and Prebiotics, a true postbiotic must include inactivated microbial components, not just purified metabolites like isolated butyric acid [2]. Interestingly, even probiotic supplements often contain a significant portion of dead cells - estimated at 10% to 30% - which still provide health benefits. This highlights the therapeutic potential of postbiotics as a stand-alone option [2].
Let’s break down what makes up these powerful compounds.
Main Components of Postbiotics
Postbiotics can be grouped into two main categories: structural components and metabolic byproducts.
- Structural components: These include inactivated microbial cells (whole or fragmented), cell wall elements like peptidoglycan and teichoic acids, and surface proteins. These parts can stimulate immune responses and help strengthen the gut lining.
- Metabolic byproducts: These are the compounds produced during fermentation. Key players include short-chain fatty acids (SCFAs) like butyrate, acetate, and propionate, which fuel colon cells and reduce inflammation. Other examples are exopolysaccharides, which have antioxidant properties and can block harmful biofilms, and bioactive peptides that may help regulate blood pressure. Postbiotics may also contain vitamins (like B-group vitamins and vitamin K), enzymes that combat oxidative stress, and organic acids that promote a balanced gut environment [2].
| Component Type | Examples | Primary Biological Role |
|---|---|---|
| Short-Chain Fatty Acids | Butyrate, Acetate, Propionate | Provide energy for colon cells and reduce inflammation |
| Cell Wall Components | Teichoic acid, Peptidoglycan | Boost immune responses and strengthen the gut barrier |
| Exopolysaccharides | Kefiran, β-glucans | Act as antioxidants and prevent harmful biofilm formation |
| Bioactive Peptides | VPP, IPP, p40, p75 | Support gut lining integrity and may regulate blood pressure |
| Vitamins | B12, B2, B6, B9, K | Aid in cellular functions like DNA replication and clotting |
Understanding these components helps explain how postbiotics contribute to gut and immune health.
How Postbiotics Work in the Body
Postbiotics support gut and immune health through several interconnected mechanisms:
-
Strengthening the Gut Barrier
Postbiotics enhance the gut barrier by regulating tight junction proteins (like occludin, claudin, and ZO-1) that keep intestinal cells tightly linked, preventing harmful substances from entering the bloodstream. They also stimulate mucin production via the MUC2 gene, thickening the protective mucus layer along the gut lining [2]. Some components, like exopolysaccharides, activate pathways such as STAT3 to boost these tight junctions, while others influence proteins through the PI3K/Akt pathway [2]. -
Immune Modulation
Postbiotics interact with immune cells in the gut to fine-tune inflammatory responses. They reduce pro-inflammatory markers (e.g., TNF-α, IL-6) and increase anti-inflammatory cytokines (e.g., IL-10), creating a balanced immune response capable of addressing threats without overreacting [2]. -
Systemic Metabolic Effects
Beyond their local effects in the gut, postbiotics influence overall metabolism. Short-chain fatty acids, for example, regulate lipid metabolism, improve insulin sensitivity, and even affect the gut-brain axis by modulating neurotransmitters. They can also enhance drug efficacy; for instance, they’ve been shown to increase the bioavailability of omeprazole by 269.9% and lurasidone by 4.3-fold by lowering intestinal pH and altering enzyme activity [2]. -
Shaping the Gut Microbiome
Postbiotics help maintain a balanced gut microbiome by lowering intestinal pH, producing antimicrobial compounds like bacteriocins, and inhibiting harmful biofilms. This creates an environment where beneficial bacteria can thrive [2].
"The viability of probiotics is a critical factor... This requirement makes them sensitive to storage conditions, including temperature and pH levels."
- Zerihun Asefa, Food Science and Nutrition Researcher [2]
How Postbiotics Restore Gut-Immune Balance
Postbiotics play a vital role in maintaining the harmony between your gut and immune system. Did you know that more than 75% of your body's lymphatic cells are located in the gut-associated lymphoid tissue (GALT)? This tissue is responsible for producing about 80% of all immunoglobulins, underscoring the deep connection between gut health and immunity [7]. Let's explore the key ways postbiotics help restore this balance.
Reducing Inflammation and Strengthening the Gut Barrier
One of the standout features of postbiotics is their ability to reduce inflammation while reinforcing the gut's protective barrier. Short-chain fatty acids (SCFAs), such as butyrate, act as fuel for colonocytes - the cells lining your colon. In turn, they strengthen the gut barrier by increasing tight junction proteins like occludin, claudin, and ZO-1 [2][9]. For example, studies on Lactiplantibacillus plantarum exopolysaccharides (EPS) have shown these compounds enhance the gut barrier by boosting ZO-1 and occludin expression while suppressing the inflammatory protein Claudin-2 [9].
Postbiotics also stimulate goblet cells to produce mucins, a key component of mucus that traps pathogens before they can harm intestinal cells. This process is driven by increased MUC2 expression through the NF-κB signaling pathway [2].
On the immune front, postbiotics encourage a shift toward balance by promoting anti-inflammatory cytokines like IL-10 and TGF-β, while reducing pro-inflammatory markers such as TNF-α, IL-6, and IL-1β [2][6]. This is crucial, considering that chronic low-grade inflammation contributes to many noncommunicable diseases, which accounted for 74% of global deaths in 2020 [2]. Additionally, postbiotics contain antioxidant enzymes like superoxide dismutase (SOD), catalase, and glutathione peroxidase (GPx), which neutralize reactive oxygen species (ROS), protecting the intestinal lining from damage [6][9].
Improving Immune Function
A stronger gut barrier sets the stage for enhanced immune performance. Postbiotics interact with immune cells like dendritic cells and macrophages, which then activate T and B lymphocytes - key players in adaptive immunity [6]. One notable mechanism involves the differentiation of regulatory T cells (Tregs) via Foxp3 expression. These specialized cells help regulate immune responses, preventing overactivity [4][8].
Postbiotics also boost the production of secretory IgA (sIgA), an antibody that captures pathogens within the mucus layer, reducing the risk of infections [4][8]. Beyond the gut, their benefits extend to the gut-lung axis. For instance, bacterial lysates - a type of postbiotic - have been shown to reduce respiratory infections in children, as confirmed by a meta-analysis of over 4,800 participants [6].
Supporting a Healthy Microbiome
Postbiotics don't just work on the immune system - they also create a gut environment that supports beneficial bacteria. SCFAs lower intestinal pH, making it harder for harmful bacteria to survive, while also improving the absorption of nutrients [2]. Additionally, postbiotics produce bacteriocins, which are antimicrobial peptides that target harmful bacteria without disrupting the good ones [2][14].
Certain components of postbiotics, like exopolysaccharides, even serve as food for beneficial bacteria, promoting their growth [2]. Through a process called cross-feeding, postbiotics containing lactate and acetate provide substrates for beneficial bacteria like Anaerobutyricum, which convert these into butyrate. This creates a self-sustaining cycle of gut health [9]. Moreover, inanimate microbial cells and their components compete with harmful bacteria for colonization sites on the intestinal lining, reducing the risk of pathogenic overgrowth [4][3].
| Postbiotic Mechanism | Primary Action | Health Outcome |
|---|---|---|
| Barrier Strengthening | Increases tight junction proteins (ZO-1, occludin) | Prevents toxins and pathogens from entering the bloodstream |
| Inflammation Control | Promotes IL-10; reduces TNF-α and IL-6 | Lowers chronic inflammation and protects tissues |
| Immune Enhancement | Activates dendritic cells and T/B lymphocytes | Strengthens pathogen defense and antibody production |
| pH Modulation | SCFAs reduce intestinal pH | Inhibits the growth of harmful bacteria |
| Antimicrobial Activity | Produces bacteriocins | Targets and suppresses harmful bacterial species |
sbb-itb-1bbfe7f
Clinical Evidence for Postbiotics
Research Studies and Findings
Recent clinical research has shed light on how postbiotics can influence inflammation and bolster gut health. For instance, an August 2021 study revealed that peptidoglycan (PG05) from Lactobacillus rhamnosus CRL1505 helped normalize inflammatory markers such as TNF-α and IL-6, while boosting beneficial markers like IL-10 and IFN-γ in protein-malnourished mice. This resulted in faster clearance of Streptococcus pneumoniae from the lungs and minimized tissue damage [17].
In March 2025, a study focused on postbiotics derived from Saccharomyces boulardii in a mouse model of ulcerative colitis. The findings highlighted a notable reduction in pro-inflammatory markers (IL-1β, IL-6, and TNF-α) and an increase in anti-inflammatory IL-10 levels [15]. Similarly, a February 2023 comparative study demonstrated that postbiotics from Bifidobacterium adolescentis B8589 provided greater modulation of gut microbiota and metabolic pathways compared to its probiotic form [16].
"Postbiotics are to be considered for use as next-generation biotherapeutics in managing ulcerative colitis or even other diseases." - Nature [16]
Postbiotic benefits extend beyond gut health. For example, topical application of bacterial lysates from Bifidobacterium longum improved reactive skin conditions by reducing vasodilation, swelling, and mast cell activation [3]. Additionally, postbiotics have shown potential in enhancing drug absorption, increasing omeprazole bioavailability by 269.9% and boosting lurasidone absorption by 4.3-fold [15]. These findings underscore the therapeutic potential of postbiotics, often surpassing traditional probiotics in effectiveness.
Postbiotics vs. Probiotics
Clinical comparisons highlight that postbiotics offer consistent benefits with fewer risks than probiotics. A key advantage is their safety - postbiotics eliminate concerns about bacterial translocation or infections, making them suitable for immunocompromised individuals [3][16].
| Feature | Probiotics | Postbiotics |
|---|---|---|
| Viability | Live microorganisms [15] | Inanimate/non-viable [16] |
| Safety Profile | Risk of infection in immunocompromised patients [16] | Safe for vulnerable populations [3] |
| Mechanism | Requires gut colonization [4] | Directly interacts with host receptors [6] |
| Gene Transfer Risk | Potential spread of antibiotic resistance genes [16] | No risk of horizontal gene transfer [16] |
| Clinical Efficacy | Variable based on viability [15] | Consistent, targeted outcomes [3] |
"The concern of probiotic viability is no longer an issue in the case of postbiotics, which has no risk in causing life-threatening conditions like bacteremia." - Nature [16]
Adding Postbiotics to Your Daily Routine
Incorporating postbiotics into your daily life can help maintain a balanced gut and immune system, building on their proven benefits.
Benefits of Synbiotics: Prebiotics, Probiotics, and Postbiotics Combined
Synbiotics combine the strengths of prebiotics, probiotics, and postbiotics into a single, comprehensive solution for gut health. Prebiotics feed beneficial bacteria, probiotics colonize the gut, and postbiotics deliver bioactive metabolites that work immediately. Together, they form a powerful trio that supports gut-immune balance more effectively than postbiotics alone [19][20].
This combination is particularly important because it addresses differences in individual gut microbiomes. Some people might not respond to a single type of biotic, but the combined approach of synbiotics helps overcome such variability [20].
The growing interest in these formulations is evident in market trends. The global market for synbiotics was valued at $57,074.2 million in 2023 and is projected to grow at a rate of 7% annually through 2030, driven by increasing clinical research and validation [19]. For example, studies show that synbiotic formulations significantly reduce pro-inflammatory markers like TNF-α and IL-1α in patients with ulcerative colitis [19]. Additionally, a study involving 137 adults with chronic diarrhea found postbiotic supplementation to be more effective than probiotics alone [23].
One standout example of this synergistic approach is Begin Rebirth RE-1™, a clinical-grade synbiotic formulation.
How Begin Rebirth RE-1™ Supports Gut-Immune Balance
Begin Rebirth RE-1™ is a 3-in-1 eubiotic synbiotic designed to quickly restore gut health. Each sachet contains 500 billion CFU of Human Origin Strains (HOSt™), which are specifically adapted to the human gastrointestinal tract for better effectiveness and tolerance.
The formulation also includes 4.5 grams of prebiotic fiber (GOS and inulin) to nourish beneficial bacteria, along with postbiotic metabolites that provide immediate therapeutic effects. Thanks to the proprietary Lyosublime™ delivery system, the product maintains its bioactivity by resisting moisture and environmental degradation, ensuring its components reach your gut intact [20][21].
Begin Rebirth RE-1™ is convenient for daily use, whether you're at home or on the go. It’s also vegan, gluten-free, dairy-free, soy-free, nut-free, and non-GMO, making it suitable for a variety of dietary needs.
Usage Guidelines and Expected Results
Begin Rebirth RE-1™ offers three tailored programs to reset your microbiome based on your health goals:
- 7-Day Rapid Reset: Designed to quickly suppress harmful pathogens and stabilize gut-immune balance. Research shows significant increases in beneficial strains like Lactobacillus and Enterococcus within just 7 days of using high-concentration formulations [4].
- 4-Week Restoration: Focuses on relieving digestive issues such as IBS, bloating, and irregular bowel movements while strengthening the gut barrier. Studies report noticeable improvements in pain and bowel regularity after 4 weeks of consistent postbiotic use [18].
- 12-Week Maintenance: Aims to sustain immune balance and promote long-term microbiome diversity, particularly for conditions like seasonal allergies or eczema. Research suggests that taking postbiotics for 8 to 12 weeks can significantly reduce symptoms and allergic reactions [18].
"Postbiotics are the endgame of probiotics and prebiotics - what they produce, which can be made into products or treatments that would have a healing effect on people." - Brian Weiner, MD, Gastroenterologist, Cleveland Clinic [18]
Experts recommend about 5 grams of prebiotics daily to properly nourish gut bacteria [22]. Begin Rebirth RE-1™ provides 4.5 grams of prebiotic fiber per sachet, aligning closely with these recommendations to support continuous metabolite production throughout each program.
Conclusion
Postbiotics offer a promising way to restore balance between the gut and immune system. These bioactive compounds - like short-chain fatty acids, proteins, and cell fragments - help strengthen the gut barrier, regulate inflammation, and support a thriving microbiome. Unlike live probiotics, postbiotics are stable, making them a safer option for immunocompromised individuals by eliminating the risk of bacterial translocation.
The science backs this up. Chronic inflammation and gut imbalances contributed to 74% of global deaths in 2020 due to noncommunicable diseases [2]. Postbiotics work to address these issues by supporting beneficial bacteria and modulating immune responses.
"Postbiotics present a sustainable, non-viable, and functionally rich alternative to probiotics, aligning with global health goals by offering safer, scalable, and effective therapeutic solutions." - John Godwin Christopher, Department of Biomedical Sciences, Vellore Institute of Technology [14]
For those looking for a practical solution, Begin Rebirth RE-1™ offers a comprehensive formula that combines prebiotics, probiotics, and postbiotics. Each sachet includes 500 billion CFU of Human Origin Strains and 4.5 grams of prebiotic fiber, delivering the synergy needed to restore gut and immune health.
Take charge of your gut health today - whether through a 7-day reset, a 4-week restoration, or a 12-week maintenance plan - and experience the benefits of improved immunity, reduced inflammation, and better overall wellness.
FAQs
What makes postbiotics more stable and effective than probiotics?
Postbiotics are non-living bioactive compounds produced by beneficial microbes. These include peptides, short-chain fatty acids, and cell fragments. Unlike probiotics, which are live bacteria that need to survive the challenges of manufacturing, storage, and digestion to work effectively, postbiotics come with a built-in advantage: they’re naturally more stable. They can withstand heat, moisture, and pH changes, meaning they don’t require refrigeration and are easy to store.
When it comes to benefits, probiotics rely on live bacteria successfully interacting with the gut, which can vary depending on a person’s unique microbiome. Postbiotics, however, skip this uncertainty by delivering their bioactive compounds directly. This makes their effects on gut and immune health more consistent and predictable. Begin Rebirth RE-1™ combines postbiotics with prebiotics and probiotics to support gut-immune balance in a way that’s both effective and reliable.
What are the health benefits of adding postbiotics to my routine?
Adding postbiotics to your daily regimen can do wonders for your gut and immune health. These bioactive compounds, created by probiotics, play a key role in fortifying the intestinal barrier. This helps reduce "leaky gut", preventing harmful substances from slipping into your bloodstream. Postbiotics also serve as immune modulators, boosting your body’s natural defenses while easing chronic inflammation - potentially lowering the risk of infections and autoimmune concerns.
But that’s not all. Postbiotics bring antioxidant power to the table, helping to fight oxidative stress, which contributes to aging and chronic conditions like cardiovascular disease, type 2 diabetes, and obesity. They may also provide antimicrobial support, improve metabolic health by regulating glucose and lipid levels, and even enhance mental well-being by building resilience to stress.
Looking for an easy way to get started? Begin Rebirth RE‑1™ offers a convenient solution by combining prebiotics, probiotics, and postbiotics in one sachet. Its advanced delivery system ensures your body absorbs these benefits effectively, helping you restore gut balance in just 7-day, 4-week, or 12-week protocols.
Are postbiotics safe to use, and are there any side effects?
Postbiotics are widely regarded as safe since they don’t contain live microorganisms. This eliminates the risk of infections that can sometimes arise with probiotics. Because they are non-living, they tend to be a lower-risk option for most people.
That said, some individuals might notice mild side effects like bloating, gas, or even allergic reactions - especially those with sensitive digestive systems or compromised immune health. Serious reactions are uncommon, but if you have any underlying health issues or specific concerns, it’s always smart to check in with a healthcare professional.
If you're searching for a dependable postbiotic option, Begin Rebirth RE-1™ is worth considering. This product combines prebiotics, probiotics, and postbiotics in a clinically-supported formula. By avoiding live organisms, it further reduces potential risks while promoting gut and immune health.