Exercise and gut health are deeply connected. Regular physical activity can improve your gut microbiome, which affects everything from digestion to immunity and even mental health. Here's what you need to know:
- Exercise boosts gut diversity: More bacterial species in your gut mean better metabolism and reduced inflammation.
- Moderate exercise is key: Activities like brisk walking or swimming for 30–60 minutes can strengthen your gut lining, improve immune function, and increase beneficial bacteria.
- High-intensity workouts need caution: Training too hard without recovery can temporarily weaken your gut barrier and cause inflammation.
- Gut microbes help performance: Certain bacteria produce compounds like short-chain fatty acids (SCFAs) that fuel muscles and reduce inflammation.
To maximize the benefits, combine consistent exercise with a fiber-rich diet to nourish gut bacteria. Stay hydrated, avoid overtraining, and consider probiotics if you're increasing workout intensity. A balanced routine supports your gut and overall health.
Gut Talk: Is Exercise Good For the Gut Microbiome?
How Exercise Influences the Gut Microbiome
Exercise sets off a chain reaction of metabolic and immune responses that reshape the gut microbiome. These changes happen through three main pathways: increasing microbial diversity, boosting the production of helpful metabolites, and strengthening the immune system within the gut. Together, these processes show how physical activity and gut health are closely connected.
Increased Microbial Diversity
Consistent exercise changes the composition of gut bacteria, increasing what's known as alpha diversity. This term refers to both the variety of bacterial species and their balanced distribution - key indicators of a healthy gut microbiome [2][6]. Regular activity encourages the growth of beneficial bacteria like Bacteroidetes, Bifidobacterium, and Faecalibacterium prausnitzii, while reducing pro-inflammatory groups such as Proteobacteria [2][1].
Studies highlight this effect in elite athletes. For example, rugby players were found to host 22 bacterial phyla in their gut compared to only 11 in sedentary individuals. Similarly, swimmers participating in a 7-week high-intensity interval training (HIIT) program showed notable increases in alpha diversity [1][2].
Exercise also impacts the Firmicutes:Bacteroidetes (F:B) ratio, a marker tied to metabolic health. Physical activity typically lowers this ratio, which has been associated with better metabolism and reduced obesity risk [6][1]. This happens partly because exercise triggers the release of compounds like lactate, which bacteria such as Veillonella convert into short-chain fatty acids (SCFAs), beneficial for overall gut health [2][3]. High microbial diversity has been linked to lower risks of metabolic syndrome, cardiovascular disease, obesity, and even depression [2].
Interestingly, combining aerobic and resistance training seems to enhance alpha diversity more effectively than resistance training alone [2][6]. With approximately 160 bacterial species living in the large intestine - amounting to over 3.3 pounds of biomass - exercise plays a key role in maintaining this ecosystem.
Metabolic Pathways and Short-Chain Fatty Acids (SCFAs)
Greater microbial diversity paves the way for increased SCFA production, essential for gut energy and inflammation control. During exercise, gut bacteria ramp up their production of SCFAs like butyrate, propionate, and acetate. These are created when microbes ferment undigested fibers and certain peptides in the colon [3]. But SCFAs aren't just byproducts - they act as signaling molecules that fuel gut cells and regulate inflammation.
Physical activity promotes the growth of butyrate-producing bacteria, including Roseburia, members of the Lachnospiraceae family, Faecalibacterium prausnitzii, and others in the Clostridiales group [3][6]. Butyrate is especially important as it powers colonocytes (the cells lining the colon) and helps maintain the gut's protective mucosal barrier [3]. For instance, professional rugby players have been found to have higher levels of fecal SCFAs and more active carbohydrate metabolic pathways compared to less active individuals [6][5].
Veillonella bacteria, which convert lactate into SCFAs, play a role in improving endurance. Typically, SCFAs appear in a 60:20:20 ratio for acetate, propionate, and butyrate, and together they provide about 10% of the body's total energy needs [3]. A study involving a 6-week endurance exercise program in lean adults revealed a significant increase in fecal SCFA levels, though these gains disappeared once the program ended [3].
| SCFA Type | Primary Role in Gut Health | Exercise Impact |
|---|---|---|
| Butyrate (C4) | Fuels colonocytes, reduces inflammation, strengthens gut lining | Increased by moderate-to-vigorous exercise |
| Propionate (C3) | Supports liver gluconeogenesis, converted from lactate by Veillonella | Rises during and after high-intensity endurance events |
| Acetate (C2) | Provides systemic energy, regulates gut pH to block pathogens | Linked to overall microbial diversity |
Gut-Immune System Interactions
Exercise doesn't just change the makeup of gut bacteria - it also influences how the gut interacts with the immune system. Moderate physical activity activates gut-associated lymphoid tissue (GALT), improving immune surveillance and balancing inflammation, both of which are crucial for a healthy microbiome [8].
When you exercise, your muscles release signaling molecules called myokines, such as interleukin-6 (IL-6). IL-6 triggers an anti-inflammatory response, boosting the production of IL-10 and IL-1ra while suppressing harmful cytokines like TNF-α [1][8]. SCFAs also play a role here, with butyrate helping to develop regulatory T cells (Tregs), which are vital for immune balance [2]. Exercise further reduces inflammation by suppressing the Toll-like receptor 4 (TLR4) pathway, which otherwise reacts to harmful lipopolysaccharides (LPS) leaking through a weakened gut barrier [1].
Moderate-intensity continuous training (MICT) has shown to increase tight junction proteins like ZO-1 and occludin by 15% to 20%, effectively sealing gaps between intestinal cells and preventing harmful substances from entering the bloodstream [8]. This type of exercise also raises levels of intestinal immunoglobulin A (IgA), which strengthens resistance to pathogens and supports beneficial bacteria [8][1].
"A bidirectional gut‐exercise axis emerges, with MICT linked to IBS symptom relief and reduced colitis severity in trials." - Springer Nature Link [8]
MICT can increase microbial alpha diversity by 10% to 20% over 8 to 12 weeks while also reinforcing the gut barrier and lowering oxidative stress. However, balance is key. High-intensity exercise lasting more than 90 minutes at over 70% VO2 max can temporarily increase gut permeability in 20% to 30% of untrained participants [8]. Finding the right mix of intensity and duration is essential for optimizing the gut-immune connection.
Exercise Intensity and Gut Health Outcomes
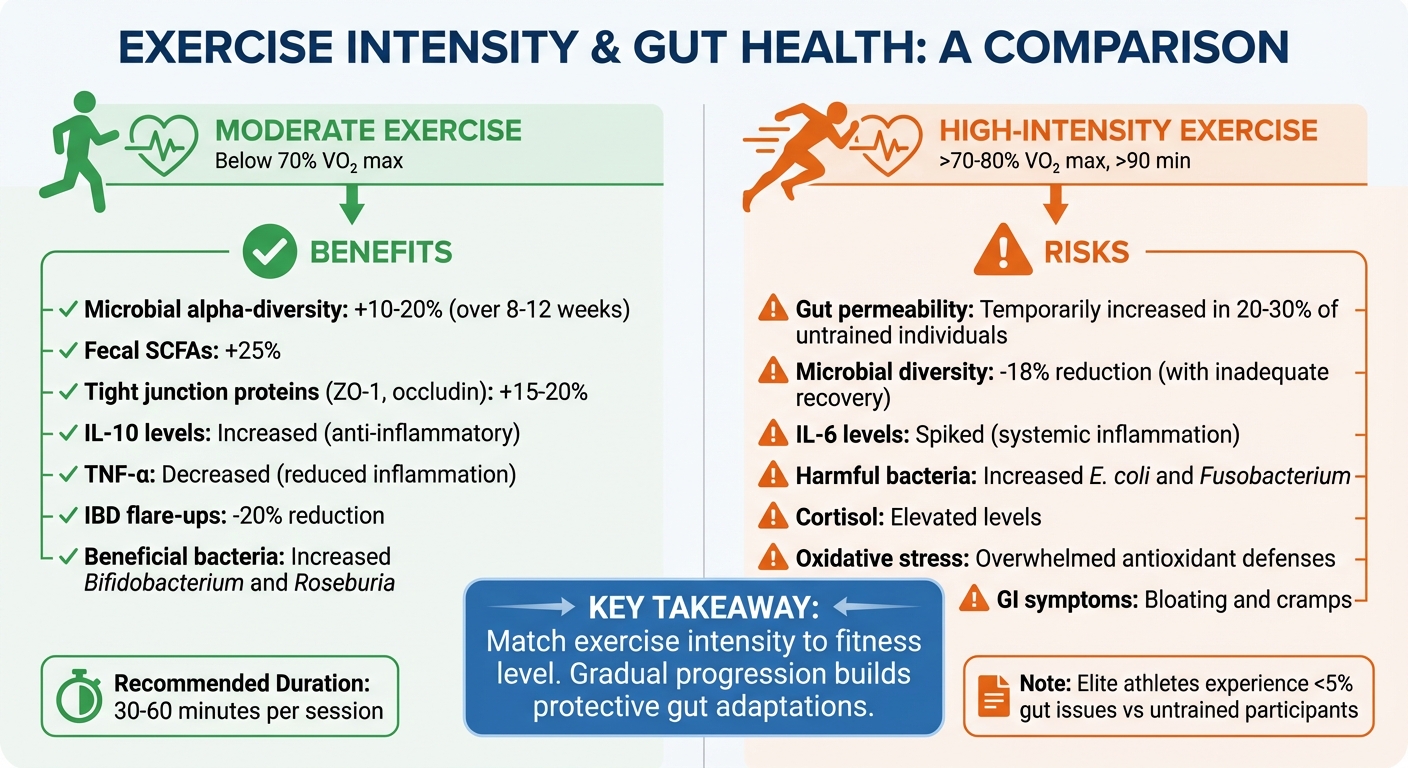
Moderate vs High-Intensity Exercise Effects on Gut Health
Exercise intensity plays a key role in shaping gut health. By understanding how different levels of exercise impact the gut, you can harness the benefits while steering clear of potential drawbacks.
Moderate Exercise Benefits
Moderate-intensity exercise - defined as activity below 70% of your maximum oxygen uptake (VO₂ max) - has been shown to improve gut health significantly. Over 8 to 12 weeks, it can boost microbial alpha-diversity by 10% to 20% and increase fecal short-chain fatty acids (SCFAs) by 25% [8]. These changes occur because moderate activity enhances blood flow to the intestines, delivering much-needed oxygen and nutrients to support beneficial bacteria.
This level of exercise also strengthens the gut barrier by improving tight junction integrity [8]. A stronger gut barrier helps prevent harmful substances from leaking into the bloodstream, a condition often referred to as "leaky gut." Additionally, moderate exercise promotes an anti-inflammatory state by increasing IL-10 levels while reducing TNF-α, two key immune markers [8].
"The bidirectional relationship between physical activity and the gut microbiome is exemplified by how exercise can promote beneficial bacteria while a healthy gut microbiome can potentially enhance exercise ability through various mechanisms." - Sanish Varghese, Department of Biochemistry, Weill Cornell Medicine–Qatar [2]
Moderate exercise also encourages the growth of beneficial bacteria like Bifidobacterium and Roseburia, which produce butyrate - a compound that nourishes colon cells and reduces inflammation [8]. Clinical studies have linked moderate exercise to a 20% reduction in inflammatory bowel disease flare-ups [8].
High-Intensity Exercise Risks
High-intensity exercise, especially when exceeding 70% to 80% VO₂ max for sessions longer than 90 minutes, can shift the effects on gut health from positive to potentially harmful. Activities like high-intensity interval training (HIIT) and extended endurance workouts redirect blood flow away from the gut to fuel working muscles. This reduced blood flow, known as splanchnic hypoperfusion, deprives the gut of oxygen, leading to oxidative stress and damage to the intestinal lining [8][9].
In 20% to 30% of untrained individuals, intense exercise temporarily increases gut permeability, allowing bacterial toxins like lipopolysaccharides (LPS) to enter the bloodstream [8]. This can trigger systemic inflammation by spiking IL-6 levels [3]. Repeated high-intensity sessions without proper recovery may also reduce microbial diversity by 18% and encourage the growth of harmful bacteria like Escherichia coli and Fusobacterium [8].
Other risks include elevated cortisol levels and oxidative stress, which can disrupt the gut-brain axis and overwhelm the body's natural antioxidant defenses [8][9]. Symptoms like bloating and cramps often follow [7]. However, highly trained athletes experience far fewer gut issues - less than 5% - compared to untrained participants, suggesting that gradual fitness progression fosters protective adaptations [8].
To minimize these risks, it's crucial to match your exercise intensity to your fitness level. Avoid prolonged sessions above 80% VO₂ max, stay hydrated to maintain intestinal blood flow, and allow for adequate recovery between high-intensity workouts [8]. Pairing intense training with proven gut health strategies can also help stabilize your microbiome and manage inflammation during demanding periods.
These findings highlight the importance of tailoring exercise intensity to support gut health. By understanding how different levels of physical activity influence your gut and immune system, you can create a balanced routine that promotes overall well-being.
sbb-itb-1bbfe7f
Long-Term Gut Changes in Athletes
Extended periods of intense exercise lead to lasting changes in the gut, which can boost both athletic performance and recovery.
Microbiome Diversity in Athletes
Elite athletes tend to have a gut microbiome that's far more diverse than that of sedentary individuals. A 2014 study comparing 40 male professional rugby players with 46 healthy controls found that the athletes' gut microbiomes included 22 distinct phyla, 68 families, and 113 genera - nearly double the diversity observed in non-athletes [1].
"Athletes had a higher diversity of gut microorganisms, representing 22 distinct phyla." - Clarke et al. [9]
Certain beneficial bacteria thrive in the guts of athletes. For example, Akkermansia muciniphila and Veillonella atypica are more abundant. Interestingly, Veillonella atypica plays a key role in converting lactate produced during exercise into propionate, which may help improve endurance. One study on Boston Marathon runners revealed that isolating Veillonella and administering it to mice increased their treadmill exhaustion time by 13% [11].
The gut microbiome of athletes also shows functional advantages. Enhanced metabolic pathways related to amino acid synthesis, carbohydrate metabolism, and fiber fermentation are common. For instance, professional cyclists exhibit higher levels of Methanobrevibacter smithii transcripts compared to amateur cyclists, reflecting adaptations to meet their intense energy demands. Furthermore, athletes produce greater levels of fecal short-chain fatty acids (SCFAs), which are essential for gut health and energy production [6].
These microbial shifts highlight the potential for further gut optimization through tailored diets and training regimens.
Diet, Fitness, and Gut Health Connections
While exercise significantly impacts gut health, dietary habits play an equally important role in shaping the athletic gut microbiome. The combination of intense training and targeted nutrition creates a unique microbial environment. High protein intake, for example, is a common feature in athletes' diets. In the Irish rugby study, athletes derived about 22% of their total energy from protein, a factor linked to their enhanced microbial diversity [11].
Cardiorespiratory fitness also influences the gut microbiome. Athletes with higher VO₂ max levels tend to have a greater Firmicutes-to-Bacteroidetes ratio and a more diverse microbial population [3]. In professional cyclists, the abundance of Prevotella (≥2.5%) was directly tied to the number of weekly training hours, demonstrating how training volume can drive microbial changes [3]. A 2023 study by Kulecka et al. further highlighted the distinct gut profiles of endurance athletes, identifying 45 bacterial species that set them apart from esports players [11].
Training cycles, or periodization, also affect gut health. During intense preparation phases, athletes typically show increased levels of Bifidobacterium and Alistipes. However, these changes are temporary - when training stops, the gut microbiome often reverts to its original state within weeks [3].
| Feature | Elite Athletes | Sedentary Individuals |
|---|---|---|
| Microbial Diversity | 22 distinct phyla, 68 families, 113 genera [1] | 11 phyla, 33 families, 65 genera [1] |
| Key Beneficial Bacteria | Higher levels of Akkermansia, Veillonella, Faecalibacterium [9] | Lower levels of health-associated species [9] |
| SCFA Production | Higher levels of butyrate and propionate [6] | Lower SCFA concentrations [6] |
| Metabolic Focus | Enrichment in amino acid synthesis and lactate utilization [3] | Standard nutrient metabolism [3] |
| Protein Intake | ~22% of total energy [11] | Typically lower |
How to Support Gut Health Through Exercise
Understanding the science behind gut health is just the start - putting it into action is where the real benefits come in. The key lies in finding an exercise routine that fits into your life while supporting your microbiome.
Finding the Right Activity Level
To promote gut health, aim for 30–60 minutes of moderate-intensity exercise at 50–70% of your maximum effort. Activities like brisk walking, swimming at a steady pace, or casual cycling are great options. Studies suggest this level of exercise can improve microbial diversity by 10–20% within 8–12 weeks and increase gut barrier proteins like ZO-1 and occludin by 15–20%, which are vital for maintaining a healthy intestinal lining [8].
"Moderate-intensity exercise has been shown to promote microbial diversity, strengthen intestinal barrier function, and exert anti-inflammatory effects, thereby supporting gut homeostasis." - Journal of Translational Medicine [8]
High-intensity interval training (HIIT) can also enhance gut diversity, but it comes with a caveat. Workouts lasting over 90 minutes at intensities above 70–80% VO₂ max could temporarily increase gut permeability. To avoid this, keep HIIT sessions shorter and less intense [7][8].
For women, exercising at least three hours per week has been linked to higher levels of beneficial butyrate-producing bacteria, such as Faecalibacterium prausnitzii and Roseburia hominis [5]. But remember, consistency is key - gut-related benefits from exercise often fade if you stop training [4][10].
Once you’ve established a workout routine, it’s time to pair it with the right nutrition to amplify the results.
Pairing Exercise with Gut-Friendly Nutrition
Matching your exercise with gut-supportive nutrition is the next step. For workouts lasting over an hour, consuming carbohydrates can help protect your gut lining. This is especially important since about 68% of athletes experience mild endotoxemia - caused by increased gut permeability - when exercising above 70% VO₂ max [3].
A high-fiber diet is essential for feeding the short-chain fatty acid (SCFA)-producing bacteria that exercise naturally enhances. These bacteria ferment fiber into SCFAs, which provide about 10% of your daily energy [3][4]. On the flip side, low-carb, high-fat diets during intense training might reduce beneficial bacteria like Faecalibacterium [3].
Protein choices also matter. Whey protein hydrolysate, for example, has been shown to lower small intestine permeability during heat stress compared to just drinking water [3]. Staying hydrated is equally important, as dehydration can disrupt blood flow to the gut, leading to gastrointestinal discomfort and microbiome imbalances [3][12].
Consider Clinically-Backed Gut Health Solutions
For those increasing their training intensity or recovering from workouts, extra gut support can make a difference. A product like Begin Rebirth RE-1™ offers a 3-in-1 synbiotic solution, combining prebiotics, probiotics, and postbiotics to help restore microbiome balance. With 500 billion CFU per serving and Human Origin Strains (HOSt™), it’s designed to complement your exercise routine by supporting gut barrier integrity and immune health.
It also includes 4.5g of fiber (from GOS and Inulin) to boost SCFA production - the same beneficial compounds your body naturally produces during moderate exercise. Thanks to its Lyosublime™ system, it ensures optimal absorption without needing refrigeration. Available in 7-day, 4-week, and 12-week programs, Begin Rebirth RE-1™ provides tailored support whether you're starting a new fitness routine or fine-tuning athletic performance.
Research shows that pairing probiotics with exercise can reduce inflammation, minimize gastrointestinal issues, and even improve athletic performance [2]. Combining a structured workout plan with targeted microbial support creates a powerful synergy that benefits both your gut and overall health [12].
Conclusion
Exercise has a profound impact on both your microbiome and immune system. Engaging in moderate-intensity exercise can increase microbial diversity by 10–20% within 8–12 weeks. It also strengthens the gut barrier by boosting tight junction proteins, which helps maintain a balanced and resilient microbial environment [8][12].
This healthier microbiome, in turn, supports your physical performance. Exercise encourages the growth of beneficial bacteria such as Akkermansia muciniphila and Faecalibacterium prausnitzii. Meanwhile, a well-balanced gut microbiome enhances your exercise capacity by improving nutrient absorption and energy production [13]. This creates a feedback loop where both your athletic ability and metabolic health benefit [8][13].
"The bidirectional relationship between physical activity and the gut microbiome is exemplified by how exercise can promote beneficial bacteria while a healthy gut microbiome can potentially enhance exercise ability through various mechanisms." - Nutrients Journal [13]
However, exercise intensity plays a critical role. While moderate exercise reliably supports gut health, high-intensity training demands caution. Around 20–30% of untrained individuals may experience temporary gut permeability after intense workouts lasting over 90 minutes at 70–80% VO₂ max [8]. That doesn’t mean avoiding tough workouts - it’s about balancing intensity with recovery, staying hydrated, and prioritizing gut-friendly nutrition.
FAQs
How does the intensity of exercise impact gut health?
The intensity of your workouts can significantly influence your gut health. Moderate-intensity activities, such as brisk walking or cycling, are known to strengthen gut barrier function. They do this by enhancing tight junction proteins, which help maintain the integrity of your intestinal lining. Plus, these exercises create an anti-inflammatory environment, lower oxidative stress, and encourage a well-balanced and diverse gut microbiome.
However, high-intensity or prolonged strenuous exercise, particularly under extreme conditions, can have a different effect. It may temporarily increase gut permeability, which could lead to mild gastrointestinal discomfort. While these changes are usually short-term, consistently pushing your body without adequate recovery might disrupt the balance of your gut microbiota.
Striking the right balance is essential. Incorporating regular moderate exercise into your routine is one of the most effective ways to promote both gut health and overall wellness.
How do short-chain fatty acids (SCFAs) impact exercise performance?
Short-chain fatty acids (SCFAs) are created when gut bacteria digest dietary fiber, and they have an essential role in boosting physical performance. Key SCFAs like acetate, propionate, and butyrate assist in regulating energy metabolism in skeletal muscles, potentially improving endurance and athletic capacity.
These compounds enhance how efficiently the body uses energy and help reduce inflammation, which can lead to better recovery and consistent performance during exercise. Keeping your gut microbiome balanced - whether through diet, exercise, or specific interventions - can support SCFA production and align with your fitness goals.
Can the right diet boost the gut health benefits of exercise?
Yes, combining the right diet with regular exercise can do wonders for your gut health. Eating foods high in fiber, prebiotics, and fermented foods helps feed the good bacteria in your gut. This, in turn, boosts bacterial diversity and encourages the production of short-chain fatty acids (SCFAs). These SCFAs play a key role in strengthening the gut lining, calming inflammation, and supporting your immune system.
Adding consistent physical activity to the mix takes things a step further. Together with a balanced diet, exercise can help regulate energy levels, improve digestion, and even minimize any stomach issues related to working out. Prioritizing whole, nutrient-packed foods and incorporating probiotics into your meals can make your gut even more responsive to exercise, enhancing its benefits for your overall health.